The
Behavioral Interventions for Smoking Cessation
By:
Dr. Mohammed H. AL-Doghether 
ABFM, SBFM.
Consultant family medicine
Director of Center of Postgraduate
Studies in Family Medicine
Ministry of Health
Abstract:
Tobacco dependence is a chronic condition that usually requires repeated
intervention.
Effective interventions can produce long-term cessation of up
to double the rate achieved by smokers without treatment. Because
of the potential health benefits and availability of effective interventions,
every smoker should be offered these effective interventions. The
identification of smoking status and the provision of brief advice
independently increase cessation rate compared to no intervention
and should be routine as part of each contact with health services.
Interventions involving individual, group or proactive telephone counselling
are more effective than no intervention .There is a strong dose response
between the intensity (number and length of sessions) of tobacco cessation
counselling and its effectiveness . This review article provides recommendations
for practitioners to assist them in management of patients engaged
in smoking cessation.
Magnitude
of the problem
International studies indicate that one in two people who smoke long
term die early due to smoking, with half of these deaths occurring
in middle age (1)
. As well as causing premature death, use of tobacco greatly diminishes
quality of life(2),
and this affects family, friends and colleagues, as well as smokers
themselves.
Tobacco smoking also places a huge financial drain on the community.
Saudi Arabia currently imports more than 20,000 million cigarettes
annually, costing $351.8 million (ranked 10th in the world in terms
of expenditure on cigarettes)(3).
These costs do not include health care expenditure, lost productivity,
costs of tobacco addiction prevention and treatment as well as a number
of other indirect costs, which are bound to be high.
Health effects of smoking
Tobacco smoking is a major risk factor for a range of diseases and disabling
conditions. These include cardiovascular disease and stroke and many cancers,
including cancers of the lung, throat, cervix, bladder and tongue(4).
Smoking adversely affects male impotence, and women who smoke can suffer
reduced fertility and/or menstrual problems. Smoking during pregnancy
increases risks of miscarriage, premature labour, stillbirth, complications
during labour and low-birth weight babies(4)
.
Tobacco smoke also affects the health of non-smokers. Passive smoking
(environmental tobacco smoke) can cause cardiovascular disease, lung cancer,
respiratory tract irritation, and an increased risk of bronchitis, pneumonia,
asthma onset in children and increased frequency and severity of asthma
symptoms and sudden infant death syndrome(4,5).
Smoking
rates and trends in smoking in Saudi Arabia
Tobacco use is surprisingly prevalent, given the public's awareness of
those dangers. Smokers represent 21 per cent of the male population over
15 years of age.
The highest rate of smoking is amongst 21 to 40 year olds (67%). The majority
of smokers (59 per cent) smoke more than 20 cigarettes per day, and 25
per cent smoke 10 to 19 cigarettes per day. Twenty
one per cent of smokers had smoked for 20 years or more (6).The
proportion of regular smokers declined in most of western countries with
the introduction of guidelines for health clinicians and patient-centered
activities (7).
Nicotine
dependence
Nicotine is the primary substance found in tobacco that causes dependence
on cigarette smoking (8).
Nicotine reaches the brain very quickly and rapidly accumulates there
once absorbed. It works by stimulating release of dopamine, the chemical
responsible for positive mood. The acute effects of nicotine dissipate
quickly, causing decreased positive mood. As nicotine deprivation occurs,
cravings occur causing the smoker to want another cigarette to maintain
the pleasurable effects and to prevent withdrawal symptoms such as insomnia,
anxiety, anger, restlessness and increased appetite. Withdrawal symptoms
commonly occur within 12 hours of cessation, peak at three to four days,
but may persist for several weeks (9).
The
process of smoking cessation
Tobacco dependence is a chronic condition that for the majority of smokers
requires repeated and persistent effort to overcome. Theoretical analysis
of smoking cessation suggests that it is a process, not a single event
(10).
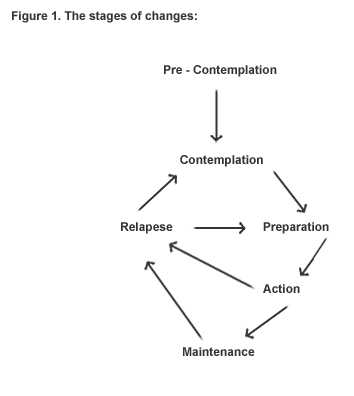
Stage of change theory (figure 1) suggests
that smokers move from being content to smoke, thinking about quitting,
planning to quit, attempting to quit, maintaining cessation or relapsing
to smoking. Smokers may cycle through some or all of the stages many times
before they achieve long-term cessation.
 |
North
American surveys suggest that two thirds of smokers are interested in
quitting but only 20 per cent are planning to quit in the next month(11)
. Overall, almost 50 per cent of smokers try to quit each year (12)
but 75 to 80 per cent of smokers that try to quit relapse within six months
and 90 per cent within 12 months (13).
Those who quit for longer may relapse at any time, even after years (14)
.
Despite the difficulty of quitting, three to five per cent of smokers
quit each year for a year or longer. Self-reported data from the US in
1997 suggest that 50 per cent of people who ever smoked successfully quit
smoking
(9).
In
the past, up to 90 per cent of smokers who successfully quit smoking did
so 'on their own'. Current estimates are that 20 to 35 per cent of quit
attempts in the United States are associated with medication use or other
forms of assistance (15,16).
The success rate of those who use some form of assistance is double (20%
vs. 8%) than of those who try to quit 'on their own' (16)
. These forms of assistance are Behavioural interventions, Pharmacological
aids or some other forms of interventions.
In this review article outlines the effectiveness and appropriateness
of Behavioural interventions for smoking cessation that can increase the
likelihood of successful smoking cessation.
Behavioural
interventions:
They consist of; self-help intervention, minimal clinical intervention
and intensive clinical intervention.
1.Self
help interventions for smoking cessation
Self-help cessation materials are a common component of most smoking cessation
interventions, ranging from brief clinical interventions to community
campaigns, but their effectiveness is not often evaluated due to practical
difficulties in 'real world settings'. In particular, there are difficulties
with follow-up of recipients and in disentangling the effects of a self-help
resource from the effects of other cessation intervention components (9,17).
There
are also difficulties in generalizing about the efficacy of a particular
method due to the lack of standardization of content (e.g. self-help manuals(18)).
Most
commonly, self-help materials are printed leaflets or manuals, although
use of audiotapes and videotapes is also well established. The new generation
of self-help materials is computer-based on CDs or internet websites or
linked to television programs.
Other forms of behavioural interventions that are predominantly self-help
are client-initiated telephone quit lines and Quit-and-Win competitions.
Quit-line services provide a contact point for provision of written self-help
materials and may also employ counsellors to assist and support people
during cessation attempts. The quit-line number is promoted extensively.
The
key elements for an effective quit-line are public access, quit smoking
resources and information, counselling, training of counsellors and referral
services (19,20).
Quit-lines are difficult to evaluate using randomized, controlled methods
because self-selection by users is part of the method and identification
and enrolment of suitable controls is difficult.
Well-promoted quit-lines
should be developed to support self-help cessation attempts.
Evidence proved that generic self-help materials alone are of small benefit
compared to no intervention as provision of self-help materials of any
type compared to no intervention, produced a small but significant increase
in the odds of quitting at six months or more (OR= 1.23, 95% CI 1.01,
1.51)(17)
.
There is not enough evidence from comparative studies to recommend one
or more types of self-help intervention over others (17).
Materials tailored to the characteristics of individual smokers (especially
stage of change) were more effective than standard materials in achieving
sustained cessation at six months (OR 1.51, 95% CI 1.13, 2.02)
(17,20,21).
A brief leaflet is sufficient to support pharmacotherapy or smoking cessation
advice from a health professional. Therefore, self-help materials should
be tailored to the needs and cessation stages of individual smokers and
selected population groups (pregnant women, asthmatics and adolescents).
2.Minimal
clinical intervention
Minimal clinical intervention, or brief advice by health professionals
could have a great influence on Saudi smoking cessation levels, but has
been underused.
Australian
doctors identify two thirds of their patients who smoke but advise only
half of these (34%) to quit (22,23).
Dentists also have high potential to provide advice on smoking cessation.
Nurses usually have frequent, more extended contact with clients/patients
so, therefore are well placed to provide cessation advice.
The US(12)
, and UK (24)
smoking cessation guidelines for health professionals recommend that all
clinicians strongly advise their patients to quit smoking.
Minimal
clinical intervention consists of brief cessation advice from health care
providers delivered opportunistically during routine consultations to
smokers whether or not they are seeking help with stopping smoking. Brief
opportunistic advice typically involves asking patients about their current
smoking, advising them to stop, offering assistance either by providing
further advice, a referral to a specialist service, or recommendation
of or a prescription for pharmacotherapy, and arranging follow up where
appropriate. This approach has been described as the 5As interventions
(table 1). The duration of each session of minimal intervention is usually
three to five minutes, and certainly less than ten minutes (25).
|
Table
1 : Minimal Clinical Interventions involve (5As):
Ask about tobacco use - doubles the rate of clinicians'
intervention.
Advise
to quit - (brief advice 3-5 min by doctor increase abstinence rate
by 10.2%at >5 months (vs. 7.9% without advice)).
Assess willingness to quit - as motivation and readiness
to quit increased abstinence rate.
Assist
in quitting - by a quit plan (STAR-P)
· Set a quit date· Tell family, friends and coworkers
about quitting and request support.
· Anticipate challenges e.g. nicotine withdrawal symptoms.
· Remove tobacco products from your environment (home, car,
work).
· By recommending Pharmacotherapy.
Arrange follow-up scheduling follow-up visits improves
cessation rate and prevent relapse.
|
Barriers
to the provision of smoking cessation advice by all health professionals
should be identified and addressed. 'Lack of time' for example is often
cited as a barrier to provision of advice, yet the evidence confirms that
clients can effectively be encouraged, advised and supported to quit within
as little as 3-5 minutes of a health professional's time. Lack of perceived
skills or training is another cited barrier, but existing evidence is
mixed regarding the added benefit of intensive cessation skills training.
Lack of immediate relevance is another barrier for health care providers
who do not perceive a direct link between smoking and the reason for presentation
of their client/patient. However, smoking has such a diversity of health
effects that most health professionals will see clients who have some
smoking related health problem or complication that is relevant to their
consultation.
3.Intensive
clinical intervention
Brief advice from a heath care provider is recognized as an important
motivator for a quit attempt (9,26).
However, the 5As approaches to minimal intervention stress the importance
of assisting clients to make a cessation attempt. This may include more
intensive behavioural therapy. A range of more intensive behavioural methods
has been used in clinical settings to support patient attempts at smoking
cessation. These include:
o Individual counselling
o Supportive group sessions
o Aversion therapy
Individual
behavioural counselling
Intensive interventions by health care providers are usually defined as
those that take more than ten minutes per session (12,27,28).
The distinction between minimal and more intensive intervention becomes
somewhat blurred when the clinician provides continuing support of short
duration per session.
Individual counselling was limited to counselling provided by specialist
counsellors and not by health care providers during usual care. Counselling
was also required to be of at least 10 minutes duration. The counselling
interventions typically included the following components;
- Review of the participant's smoking history and motivation to quit;
- Help in identification of high-risk situations and smoking cues; and
- Generation of problem-solving strategies to deal with high-risk situations.
Counsellors may also have provided non-specific support and encouragement
and as well as written materials, video or audiotapes.
The effect of intensive counselling compared to minimal counselling by
a doctor was greater amongst trials with patients with, or at high risk
of, smoking related disease (29).
General practitioners appear to be more willing to give advice to stop
to smokers with smoking related diseases (30).
This is despite evidence that smokers with smoking related diseases do
not respond better to such advice than others (31).
Supportive
Group Sessions
Group therapy offers individuals the opportunity to learn behavioural
techniques for smoking cessation, and to provide each other with mutual
support. Groups may be led by professional facilitators, clinical psychologists,
health educators, nurses, doctors, or successful peers. They may be conducted
in different settings and may vary in intensity, number and duration of
sessions as well as total duration.
Suggested components of a best practice group cessation clinic program
include:
o Setting a specific quit date;
o Learning to interrupt the conditioned responses that support smoking
by self-monitoring;
o
Making plans for coping with temptations to smoke following cessation;
and
o Providing follow-up contact and social support for quitting and continued
abstinence (32).
Other
optional components are:
o Instructions for effective use of NRT.
Attendance rates of smokers invited to participate in group cessation
programs reviewed by Stead and Lancaster (2000)(33)
varied from eight to 88 per cent. Group therapy can be an effective cessation
method that should be available for those who are willing to participate.
Aversion
therapy
Adding an unpleasant (aversive) stimulus to an attractive behaviour reduces
the attractiveness and may extinguish the behaviour (34).
Aversion therapy pairs the pleasurable stimulus of smoking a cigarette
with an unpleasant stimulus, with the aim of extinguishing the urge to
smoke.
The most frequently examined procedure has been rapid smoking. 'Rapid
smoking' usually consists of asking subjects to take a puff every six
to 10 seconds for three minutes, or until they consume three cigarettes
or feel unable to continue. This is repeated two or three times, and subjects
are asked to concentrate on the unpleasant sensations it causes. Explanation
and supportive counseling is usually provided with application of the
rapid smoking technique.
Other aversive techniques include rapid puffing (smoke not inhaled), smoke
holding, excessive smoking, paced smoking, self-paced smoking, focused
smoking, covert sensitization, symbolic aversion, electric shocks administered
by therapist or subject, and behavioural treatments with bitter pills.
Each
of these methods is described in more detail by Hajek and Stead (2000)(34).
There is no evidence of benefit from aversion methods other than rapid
smoking techniques (34)
. Aversion therapy techniques are outdated and not recommended in most
countries.
Conclusion:
Nicotine dependence is a tenacious and difficult addiction to treat successfully.
Clearly, perseverance on the part of the patient and the physician is
most effective for achieving permanent abstinence. Application of effective
strategies and motivational techniques are essential for success.
References
1.
Doll R, Peto R, Wheatley K, Gray R, Sutherland I. Mortality in relation
to smoking. 40 years observations on male British doctors. BMJ.1994; 309:
901-911.
2.
Hirdes J, Maxwell M. Smoking cessation and quality of life outcomes among
older adults in the Cambell survey on well-being. Can J Public Health
1994; 85: 99-102.
3.
World Health Organization (WHO). Tobacco or health: a global status report.
Geneva: WHO, 1997, pp.19-30 , pp.261-262.
4.
Winstanley M, Woodward S, Walker N. Tobacco in Australia: facts and issues
(second edition). Victorian Smoking and Health Program: Melbourne .1995,
pp. 37-67.
5.
Rashid M, Rashid H. passive maternal smoking and pregnancy outcome in
a Saudi population . Saudi Med J. 2003; 24(3): 248-53.
6.
Jarallah JS, Al-Rubeaan KA, Al-Nuaim AA, Al-Ruhaily AA, Kalantan KA. Prevalence
and determinants of smoking in three regions of Saudi Arabia. Tob Control
. 1999; 8: 53-56.
7.
Al-Doghether MH. Do we need national guidelines for smoking cessation?
.
Ann Saudi Med. 2001; 21(12): 3-4.
8.
Stolerman IP and Jarvis MJ. The scientific case that nicotine is addictive.
Psychopharmaco. 1995; 117:2-10.
9.
US Department of Health and Human Services. Reducing Tobacco Use: A report
of the Surgeon General. Executive summary. Nicotine Tob Res. 2000; 2(4):
379-95.
10.
Prochaska JO, DiClemente CC. Stages and processes of self-change of smoking
toward an integrative model of change. J Consult Clin Psychol.1983; 51:
390-395.
11.
Etter JF, Perneger TV, Ronchi A. Distributions of smokers by stage: international
comparison and association with smoking prevalence. Prev Med. 1997; 26:580-585.
12.
Fiore MC, Bailey WC, Cohen SJ, Dorfman SF, et al. Treating Tobacco use
and dependence: clinical practice guideline. Rockville (MD): US Department
of Health and Human Services, Public Health Service. 2000, pp.9-10.
13.
Carmody TP. Preventing relapse in the treatment of nicotine addiction:
current issues and future directions. J Psychoactive Drugs. 1992; 24(2):
131-158.
14.
Cohen S, Lichenstein E, proachaska J.Rossi JS, Gritz ER, Carr CR, Orleans
CT, Schoenbach VJ. Debunking myths about self-quitting: evidence from
10 prospective studies of persons who attempt to quit smoking by themselves.
Am Psychol. 1989; 44: 1355-1365.
15.
Hughes JR. Smoking cessation. N Engl J Med. 1999; 341(8): 610-611.
16.
Zhu SH, Melcer T, Sun J, Rosbrook B, Pierce JP. Smoking cessation with
and without assistance: A population-based analysis. Am J Prev Med .2000;
18(4): 305-311.
17.
Lancaster T, Stead LF. Self-help interventions for smoking cessation.
Cochrane Database of Systematic Reviews.1, 2003. Available: http://gateway1.ovid.com/ovidweb.cgi
18.
Glynn TJ, Boyd GM, Gruman JC. Essential elements of self-help/minimal
intervention strategies for smoking cessation. Health Educ Q. 1990; 17(3):
329-345.
19.
Borland R, Balmford J, Segan C, Livingston P, Owen N. The effectiveness
of personalized smoking cessation strategies for callers to a Quitline
service. Addiction .2003; 98(6): 837-46.
20.
Zhu SH, Anderson CM, Tedeschi GJ, Rosbrook B, Johanson CE, Byrd M, et
al. Evidence of real-world effectiveness of a telephone quitline for smokers.
N Engl J Med. 2002; 347(14): 1087-93.
21.
Owen L. Impact of a telephone helpline for smokers who called during a
mass media campaign. Tob Control 2000; 9: 148-154.
22.
Wiggers JH, Sanson-Fisher RW. Practitioner provision of preventive care
in general medical consultations: association with patient educational
and occupational status. Soc Sci Med.1997; 44: 137-146.
23.
Young JM, Ward JE. Implementing guideline for smoking cessation advice
in Australian General Practice: opinions, current practices, readiness
to change and perceived barriers. Fam Pract.2001; 18(1) 14-20.
24.
West R, McNeill A, Raw M. Smoking cessation guidelines for health professionals:
an update. Thorax.2000; 55(12): 987-999.
25.
Litt J. How to provide effective smoking cessation advice in less than
a minute without offending the patient. Aust Fam Physician. 2002; 31(12):
1087-94.
26.
Kreuter MW, Chheda SG, Bull FC. How does physician advice influence patient
behavior? Evidence for a priming effect. Arch Fam Med .2000; 9(5): 426-433.
27.
Lancaster T, Stead LF. Individual behavioural counselling for smoking
cessation . Cochrane Database of Systematic Reviews.1,2003. Available:
http://gateway1.ovid.com/ovidweb.cgi
28.
Rice VH, Stead LF. Nursing interventions for smoking cessation . Cochrane
Database of Systematic Reviews.1,2003. Available: http://gateway1.ovid.com/ovidweb.cgi
29.
Silagy C. Physician advice for smoking cessation. Cochrane Database of
Systematic Reviews.1,2003. Available: http:// gateway1 .ovid.com ovidweb.cgi
30.
Coleman T, Murphy E, Cheater F. Factors influencing discussion of smoking
between general practitioners and patients who smoke; a qualitative study.
Br J Gen Pract. 2000; 50; 207-210
31.
Senore C, Battista RN, Shapiro SH, Segnan N, Ponti A, Rosso S, Aimar D.
Predictors of smoking cessation following physicians counseling. Prev
Med. 1998; 27 (3): 412-421.
32.
Fisher EB, Lichenstein E, Haire-Joshu D, Morgan GD, Rehberg HR. Methods,
successes and failures of smoking cessation programs. Annu Rev Med .1993;
44: 481-513.
33.
Stead LF, Lancaster T. Group behaviour therapy programmes for smoking
cessation . Cochrane Database of Systematic Reviews.1,2003 . Available:
http://gateway1.ovid.com/ovidweb.cgi
34.
Hajek P, Stead LF. Aversive smoking for smoking cessation. Cochrane Database
of Systematic Reviews.1,2003 Available: http://gateway1.ovid.com/ovidweb.cgi
|
![]()

