
Asia Pacific Journal of Family Medicine Volume 6 Issue 1
ORIGINAL ARTICLE
Raising institutional delivery in war-torn communities: Experience of BRAC in Afghanistan
A. Hadi, T. Rahman, D. Khuram, J. Ahmed and A. Alam
Bangladesh Rural Advancement Committee Afghanistan, Kabul, Afghanistan, 454 Butcher Street, Baharistan
Correspondence: Abdullahel Hadi, BRAC Afghanistan, 454 Butcher Street,
Baharistan, Kabul, Afghanistan
Accepted for publication 20 March 2007.
Raising institutional delivery in war-torn communities: Experience of BRAC in Afghanistan
A. Hadi, T. Rahman, D. Khuram, J. Ahmed and A. Alam
Bangladesh Rural Advancement Committee Afghanistan, Kabul, Afghanistan, 454 Butcher Street, Baharistan
Correspondence: Abdullahel Hadi, BRAC Afghanistan, 454 Butcher Street,
Baharistan, Kabul, Afghanistan
Accepted for publication 20 March 2007.
Abstract
Aims: Although reproductive health services have been expanded in rural communities in Afghanistan in the last several years, no systematic attempt has been made to assess their contribution to promote safe delivery. This study assesses the effects of the Bangladesh Rural Advancement Committee (a non-government organisation) health programme in raising institutional delivery in post-conflict traditional communities in Afghanistan.
Methods: Data for this study came from two surveys conducted by Management Science of Health/United States Agency of International Development in 2004 and 2006 in the district of Paghman in Kabul province. A total of 180 randomly selected married women who gave birth in the last 2 years preceding the survey were interviewed.
Results: Findings reveal that institutional delivery in rural communities has been increasing even in post-conflict poor rural communities. The use of services was much higher if antenatal care was provided by midwives and physicians. Intensive community mobilization, provision of free services and transport facilities at night, incentives to health providers, maintaining privacy in the delivery room and the quality of services were the key factors in raising the number of institutional deliveries.
Conclusions: The provisions of free services and incentives for health providers worked well in raising the frequency institutional delivery. Given that Afghan communities are sparsely distributed in the countryside and largely inaccessible by most modern transport, the expansion of this approach to provide institutional delivery may not be feasible at this stage. This study argues for the promotion of new approaches to maternal health by testing the cost-effective intervention models. The study concludes that an integrated approach to address health services can significantly improve access to and the utilization of institutional delivery among poor and disadvantaged communities in Afghanistan.
Key words: Afghanistan, antenatal care, community health worker, incentive, institutional delivery
Methods: Data for this study came from two surveys conducted by Management Science of Health/United States Agency of International Development in 2004 and 2006 in the district of Paghman in Kabul province. A total of 180 randomly selected married women who gave birth in the last 2 years preceding the survey were interviewed.
Results: Findings reveal that institutional delivery in rural communities has been increasing even in post-conflict poor rural communities. The use of services was much higher if antenatal care was provided by midwives and physicians. Intensive community mobilization, provision of free services and transport facilities at night, incentives to health providers, maintaining privacy in the delivery room and the quality of services were the key factors in raising the number of institutional deliveries.
Conclusions: The provisions of free services and incentives for health providers worked well in raising the frequency institutional delivery. Given that Afghan communities are sparsely distributed in the countryside and largely inaccessible by most modern transport, the expansion of this approach to provide institutional delivery may not be feasible at this stage. This study argues for the promotion of new approaches to maternal health by testing the cost-effective intervention models. The study concludes that an integrated approach to address health services can significantly improve access to and the utilization of institutional delivery among poor and disadvantaged communities in Afghanistan.
Key words: Afghanistan, antenatal care, community health worker, incentive, institutional delivery
Introduction
More than 530 000 maternal deaths occur every year in the world of which a quarter to a third of all deaths is the result of complications during pregnancy.1,2 Inequity in the distribution of this mortality is also very wide. More than 99% of maternal deaths occur in developing countries. A woman living in Africa has 200 times greater risk of dying from pregnancy-related complications than a woman living in an industrialized country.1 Although the need for reproductive health care has been widely reported, women have little access to those health services in most developing countries.3,4 This ihas direct impact on maternal morbidity and mortality.57 Community-based intervention to promote safe motherhood had been launched in many countries8,9 but the assessment of such attempts indicates that achievements were minimal.8,10 It has been found that most maternal deaths take place at home where health facilities are out of reach for pregnant women.2 Home deliveries by traditional birth attendants (TBAs) are normal for childbirth in most traditional societies. As TBAs are not trained to manage obstetric complications, maternal mortality has remained very high in those countries.11 However, some studies claim that home-based care is more cost-effective than institutional delivery services.12 Although institutional delivery is not an affordable strategy in many poor countries, current global policy focuses on the provision of skilled birth attendants and improved obstetric services to reduce maternal mortality.2 Institutional delivery in community-based obstetric care facilities was found to be effective in significantly reducing the risk of maternal mortality.11,13 Malaysia has become successful in mobilizing most of its communities and 88% of pregnant women now deliver in rural clinics, and are assured of quality of services.11 This experience demonstrates that women prefer facility-based delivery than delivering at home if free transportation is provided and quality of services is ensured.11
State of health in Afghanistan
Afghanistan is one of the poorest countries in the world with a population of 23.8 million within an area of 647 500 km2.14,15 In addition to continuing civil war for over two decades, the country suffers from enormous poverty and a devastating economy with crumbling infrastructure. It has very poor access to education, potable drinking water and opportunities for income generation.14 In rural Afghanistan, the capacity to provide health services is severely limited with very few trained medical staff to run existing health facilities. According to one estimate, there is one qualified doctor for every 50 000 people.14 One out of five children dies before the age of five years. The life expectancy at birth has been estimated at 44.5 years. Maternal mortality is considered the highest in the world with 1600 per 100 000 live births.14 One woman dies in every 30 minutes from pregnancy-related causes.14 Less than 15% of deliveries are attended by skilled health workers.14 Severe poverty, insecurity and discrimination against women has continued for decades in the rural communities. However, it is now recognized that most of these maternal deaths were unwarranted and could have been avoided by providing appropriate health services.
Community-based safe motherhood programme of BRAC
Under the Rural Extension and Community Health (REACH) program, Bangladesh Rural Advancement Committee (BRAC, a non-government organisation) has been providing Basic Package of Health Services (BPHS) in the Paghman district of Kabul province since 2004 to ensure access to health services in the area. Paghman is located 30 km west of Kabul city. Farming has been the predominant economy in the district although a large proportion of the male population frequently moves to nearby Kabul to work. The average size of the household is eight. As found elsewhere in rural Afghanistan, health conditions in this community are very poor with high mortality and morbidity. BRAC attempted to develop an integrated health network to reach the grassroots of the district. BRAC recruited community health workers (CHWs) as the frontline workforce in the villages, and community midwives as paraprofessionals to serve in the health facilities. The CHWs were illiterate, married and middle-aged women and men recruited from the local communities. They were given basic training for 6 months and routine refresher training for 1 day in each month by BRAC physicians.
The role of male CHWs was to raise awareness in the community, particularly among adult men, shura members, religious leaders and rural elites regarding the needs of reproductive health services, immunization and family planning. On the other hand, female CHWs were trained to raise health awareness among women, identify pregnant women and motivate them to receive antenatal care services, identify sick children, provide treatment of common illnesses, promote the benefits of having institutional delivery and refer complicated cases to the nearby clinics or hospitals. On average, the CHWs were expected to visit five households a day in their own villages and join 1-day refresher training each month.
Given the severe shortage of certified midwives in Afghanistan, BRAC established midwifery training schools to develop a cadre of community midwives to serve in their own communities. The midwives were the backbone of the institutional delivery services of the BRAC programme. They provided ante- and postnatal care at various health posts (the lowest level of health facility in the community) and normal deliveries at the community clinics. In addition, they promoted institutional delivery among pregnant women while providing antenatal care at the health posts.
The performance of the CHWs and midwives were routinely monitored and supervised by community health supervisors and physicians. A total of 212 CHWs, of whom 88 were male, covered 15 460 households in the district. BRAC had eight health facilities to provide institutional deliveries in the project villages.
In some health centres, BRAC ensured round-the-clock delivery services with ambulance facilities for referral cases. Cell phones were provided to the CHWs to call the ambulance any time to bring complicated pregnancy cases to the clinics in case of emergencies. After delivery in the clinics, transportation was provided free to return the mothers and newborn babies to their homes. Most importantly, the privacy of the delivery room, a very sensitive issue in the Afghan cultural context, was ensured.
The CHWs are volunteers, while the community midwives receive much smaller amounts of money as salary compared to certified midwives working in Afghanistan. Unlike experiences elsewhere, BRAC adopted an incentive system to effectively reduce the dropout of CHWs and community midwives. Both the CHWs and midwives draw respect from their own communities which motivates them to continue their services. The CHWs also serve as social marketing agents, sell health products such as oral rehydration solution packets, iodized salt, safe delivery kits and contraceptives to their clients and make profits from each of the items sold. In addition, they receive US$0.4 as a fee for referring each pregnant woman to the clinic for delivery. Although the salary of the community midwives is negligible, they receive as an incentive US$0.7 for each delivery conducted in the clinic. In addition, midwives and other clinic staff were given allowances for night duty. It has been assumed that the BRAC approach would not only be cost-effective but the quality and coverage of services would also improve. While reproductive health services have expanded in the last several years in Afghanistan, no systematic attempt has been made to assess its contribution to promote safe delivery. In this paper, the contribution of the BRAC programme in raising institutional delivery in rural Afghanistan is examined.
Materials and methods
Data
The beforeafter approach was adopted to assess the effects of programme interventions in raising the frequency of institutional delivery. Thus, the study design included baseline (2004) and end-line (2006) surveys to measure the changes in selected health indicators. This study was conducted in Paghman district which was divided into five supervisory areas for the project. In each of the five supervisory areas, all households and eligible women were listed to develop the sampling frame. The sample size was calculated as 19 women from each supervisory area who gave birth in the 2 years preceding the survey. The sample women were selected at random from each supervisory area. Thus, the sample size was (19 x 5) or 95 women for each of the baseline and end-line surveys which provided a total of 190 married women for this study. The numbers of eligible women in the supervisory areas were unequal. Weight factors therefore were calculated and applied in estimating the results. A structured questionnaire was used to collect information. The quality of data was ensured by the local vaccination service providers and key informants in the areas. The baseline survey was conducted in March 2004 while the end-line survey was carried out in the 2 years after in March 2006.
Model specification
The study estimates the changes in institutional delivery and its predictors in the communities. Among the variables considered were the place of delivery, programme period, type of facility, visit by CHW, utilization of antenatal care (ANC) and tetanus toxoid (TT) injection, distance to the facility and type of provider for ANC. BRAC programme period was categorized into 2004 and 2006. Facility type was dichotomised as basic and comprehensive care. TT coverage was dichotomized into full or partial immunization. Distance to facility was categorized as < 10 km and 10+ km. Provider of antenatal care was categorized as doctor, midwife and none. The outcome variable was the place of delivery during the last 2 years. This was dichotomised as home and health facility.
The analysis began with a description of the health facilities and providers in the study district. The changes in CHW visits, TT coverage, antenatal care, provider of antenatal care, place of delivery, attendants during delivery and delivery complications during the study period were estimated. Relative importance of the variables was estimated by multivariate analysis.16 Two models were used. In Model 1, programme period, health facility and distance to facility were included. Model 2 included these three variables and also included antenatal care provider. Odds ratios for difference, 95% confidence intervals and p-values for a two-sided test were calculated by logistic regression.
Results
Profile of the project
The profile of the health providers and facilities in the district is presented in Table 1. On average, 73 households were visited by a CHW each month and 26 CHWs were supervised monthly by one community health supervisor. A community midwife provided services to 1288 households. On the other hand, the BRAC programme had one female doctor for nearly 3865 households. Compared to that, the number of male doctors was relatively higher with one male doctor for every 1546 households. There were eight (four basic and four comprehensive) health facilities in the district. On average, each facility provided services to 1933 households per month. However, total number of beds was only 13 in these facilities. One ambulance was available to provide services in the district. The average distance to the nearest facility from home was 11.4 km.
Antenatal and delivery care
The CHWs were the key persons who worked at the grassroots to identify pregnant women, educate and motivate them to attend the antenatal care centres, and also to deliver at the clinics or hospitals. This is reflected in Table 2 which indicates that the community health workers were able to reach most (95.5%) pregnant women in 2 years, up from only 40.3%. The proportion of pregnant women who received antenatal care also rose from 37.3% to 91.2%. Only 14.9% of pregnant women received antenatal care from midwives in 2004 which rose 67.6% 2 years later in 2006, indicating a major increase in the coverage of antenatal care (p < 0.01) by the community midwives. The proportion of women who received TT injections also increased from 77.9% to 88.2% during the study period. Among the services, the coverage of maternal immunization was high compared to other components of reproductive health care. The high maternal immunization coverage indicates that reaching a larger group of pregnant women for other services was possible within the existing provision of maternal and child health services.
Institutional delivery increased from 31.3% to 55.2% (p < 0.01) during the project period (Table 3). This was much higher than the estimate found in a study conducted in a suburb of Kabul where it was found that 35% had to go to health facilities.17 The service statistics of the project suggests that only 30% of the capacity of the existing facilities were utilized. This indicates that increase in coverage is still possible. Among the providers, the role of midwives (with the help of doctors) was enhanced to manage deliveries from 17.6% to 46.3% (p < 0.01) in 2 years. This has helped to significantly reduce the birth attendance by unskilled providers such as dais (traditional birth attendants) and family members from 69.2% to 37.3%.
Complication during delivery
Table 4 shows that the proportion of pregnant women having complications during delivery was quite high in the study district, although this declined from 16.4% to 11.9% during the study period. Not only the management of complicated delivery has improved by referring these cases to clinics, the incidence of complicated delivery at home has also declined significantly from 13.4% to 1.5%, an improvement that could not happened had there been no institutional service delivery system in place.
Effects of programme on delivery care
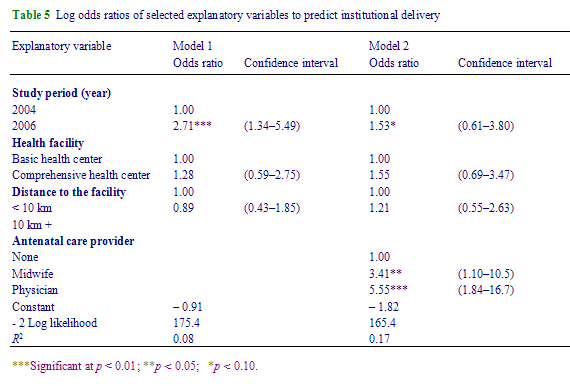
Multivariate analysis shows the net effects of the BRAC programme in raising institutional delivery (Table 5). In Model I, it appears that institutional delivery has increased 2.71 times (p < 0.01) during the study period, controlling for the role of the type of health facilities available and the distance to the facilities. When antenatal care providers were added to Model II, the effect of programme intervention in raising institutional delivery reduced to 1.53 times, indicating that antenatal care providers also had a significant role in raising institutional delivery. Clinic delivery is likely to increase 3.41 times if pregnant women receive ANC services from midwives and 5.55 times when they receive services from physicians.
Discussion
Excessive maternal deaths have never been new in Afghanistan. What is new is the recognition that most of these maternal deaths were unwarranted and could have been avoided with simple and effective health service delivery at the community level. Although reproductive health services have expanded in the last several years in Afghanistan, no systematic attempt has been made to assess its contribution to promote safe delivery. This study demonstrates that the promotion of institutional delivery is not only possible but has been on the rise even in post-conflict, poor rural communities in Afghanistan. This increase in clinic-based delivery suggests that the use of institutional delivery would increase even further if the quality of services is ensured.
In rural Afghanistan, as found in other countries as well, pregnancy and delivery are considered natural processes for a married woman rather than a condition that requires medical attention.13 Moreover, Afghan women have very limited access and exposure to modern biomedical technologies. It was therefore expected that it would be difficult to convince pregnant women and their family members to attend antenatal care and take the advantage of having clinics in their communities for delivery.
Why has institutional delivery increased so fast? It has been found that the provision of services alone cannot raise the need and utilization of services.13,18 First, effective promotion among pregnant women and their family members played a role to raise the profile of delivery at clinics.11 This community mobilization may have further accelerated by the incentives provided to the CHWs who received referral fees from BRAC for each pregnant woman.
Second, the quality of tailor-made services have attracted potential users in the communities. It seems that round-the-clock and uninterrupted services have raised the credibility of BRAC health centres. Free ambulance services, particularly at night, have not only made it possible for many to reach the centres when needed, but also ensured security for pregnant women and their attendants. Also, a normal delivery has required only 68 h in the clinic. Most Afghan families would not probably allow women to stay overnight outside home. The time needed for the services has been acceptable for them.
Third, maintenance of privacy of the delivery room has largely reduced the barrier of getting permission from families. The issue of maintaining privacy for women in public places is crucial in the Afghan context which has largely remained unnoticed by policy makers.
Fourth, it has been argued that the driving power for decisions to go to skilled providers was the fear of death during delivery.17 Afghan women learned this reality from experience. Institutional delivery was considered secure and as the last option of survival from pregnancy-related complications during deliveries by most Afghans.17
Finally, the supply-driven approach has played an important role in raising institutional delivery. The cost of delivery in the clinic or hospital was subsidized for beneficiaries. The average cost for normal delivery in BRAC facilities has been US$20 although the services have been provided free. Thus, poor Afghan families have also been able to receive these services.
BRAC has been able to create and accelerate the demand for institutional delivery services within communities. What has remained is to examine whether this approach of providing services is replicable in other places in this country. Would it be possible to institutionalize this approach within the national health care system in Afghanistan? Accessibility to services is a precondition for the utilization of institutional delivery services13,1922 and the utilization of services would depend not only on the availability and distance but also the cost and quality of services.13 Providing institutional delivery in remote villages in Afghanistan requires massive health infrastructure investments. Given that Afghan communities are sparsely distributed in the countryside and largely inaccessible by any modern transport, it may not be feasible to expand the network of institutional delivery in the countryside at this stage.
Afghanistan continues to face a formidable challenge in the improvement of maternal health for the poor living in remote communities. Maternal health services and institutional delivery should be considered as the priority needs of the population. This study argues for the promotion of new approaches of maternal health by testing cost-effective intervention models. One good strategy would be the promotion of safe delivery at home. An essential element of this strategy should be ensuring skilled birth attendants at the community level. That would require sensitization of the community about the benefits of this approach, inclusion of the stakeholders and participating non-government organizations in the relevant communities. This study concludes that an integrated approach to address health services can significantly improve access to and utilization of institutional delivery among poor and disadvantaged communities in Afghanistan.
Acknowledgments
This research was a part of the evaluation of REACH programme of MSH/USAID in Afghanistan. The author wishes to thank the MSH officials of REACH programme and the Ministry of Public Health (MoPH) of the Islamic republic of Afghanistan for their inspiration, encouragement and continued support of the study and for their invaluable contribution in designing the evaluation protocol.
References
1 World health Organization. Pregnancy exposes women in poor states to 200-fold risk of death, compared with rich ones, says WHO. Populi 2000; 27: 4.
2 Costello A, Osrin D, Manandhar D. Reducing maternal and neonatal mortality in the poorest communities. BMJ 2004; 329: 11668.
3 Cook RJ, Fathalla MF. Advancing reproductive rights beyond Cairo and Beijing. Int Fam Plan Perspect 1996; 22: 11521.
4 Hadi A. Effects of productive role of Bangladeshi women on their reproductive decisions. Asia Pac Popul J 2001; 16: 114.
5 Heise L, Moore K, Toubia N. Sexual Coercion and Reproductive Health: a Focus on Research. New York: Population Council 1995.
6 Sadik N. Human rights: women have special needs. Populi 1998; 25: 167.
7 Berer M. Safe sex, womens reproductive rights and the need for a feminist movement in the 21st century. Reprod Health Matters 2000; 8: 711.
8 Huang J, Xue Y, Jia Y, Xue J. Evaluation of a health education programme in China to increase breast-feeding rates. Health Promot Int 1994; 9: 958.
9 Tembo KC. Grass-root health education strategies in Malawi. J R Soc Health 1995; 115: 3189.
10 Laverack G, Esi-sakyi B, Hubley J. Participatory learning materials for health promotion in Ghana a case study. Health Promot Int 1997; 12: 216.
11 Koblinsky MA, Campbell O, Heichelheim J. Organizing delivery care: what works for safe motherhood? Bull World Health Organ 1999; 77: 399406.
12 Bang A, Bang R, Baitule S, Reddy M, Deshmukh M. Effect of home-based neonatal care and management of sepsis on neonatal mortality: field trial in rural India. Lancet 2000; 355: 4989.
13 Sugathan KS, Mishra V, Retherford RD. Promoting Institutional Deliveries in Rural India: the Role of Antenatal-Care Services. National Family Health Survey Report Number 20, Honolulu, East-West Center; 2001.
14 UNDP. Human Development Report 2004. New York: UNDP; 2004.
15 UNICEF. Afghanistan Progress of Provinces Multiple Indicator Cluster Survey 2003. Kabul: UNICEF, 2004.
16 Aldrich JH, Nelson FD. Linear Probability, Logit and Probit Models. Beverly Hills: Sage 1984.
17 Kaartinen L, Diwan V. Mother and child health care in Kabul, Afghanistan with focus on the mother: womens own perspective. Acta Obstet Gynecol Scand 2002; 81: 491501.
18 Ray SK, Mukhopodhyay BB, Das R, Ganguly MM, Maidal A, Roy SC. Extent of utilization of maternal health care services of PHC by families of a rural area. Indian J Public Health 1984; 28: 1227.
19 Rao PS, Richard J. Socio-economic and demographic correlates of medical care and health practices. J Biosoc Sci 1984; 16: 34355.
20 Sarita PT, Tuominen R. Use of health care services in two rural communities in Tanzania. Community Dent Oral Epidemiol 1993; 21: 1335.
21 Kumar R, Singh MM, Kaur M. Impact of health centre availability on utilization of maternity care and pregnancy outcome in a rural area of Haryana. J Indian Med Assoc 1997; 95: 44850.
22 Rohde J, Viswanathan H. The Rural Private Practitioner. New York: Oxford University Press 1995.
Table 1 Profile of health service providers and facilities

Table 2 - Antenatal care services by study period
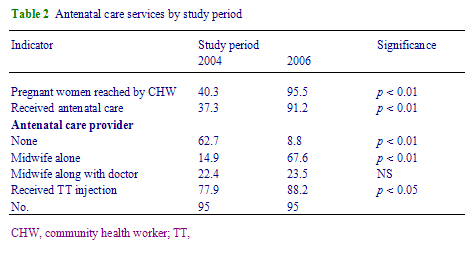
Table 3 - Providers of the delivery by the study period
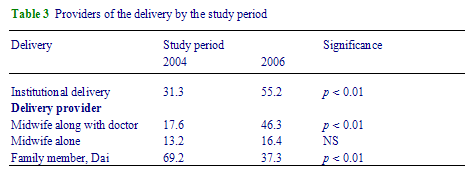
Table 4 - Complications during delivery by the place of delivery
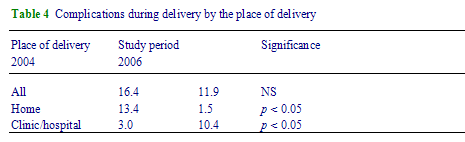
Table 5 - Log odds ratios of selected explanatory variables to predict institutional delivery
^top