
Asia Pacific Journal of Family Medicine Volume 5 Issue 3
ORIGINAL ARTICLE
Does doctorpatient stability affect the provision of good medical care?
Joachim P. Sturmberg
Department of General Practice, Monash University, Melbourne, Victoria, Australia
Correspondence: Joachim P. Sturmberg, Associate Professor of General Practice, PO Box 3010, Wamberal, New South Wales 2260, Australia.
Accepted for publication September 19, 2006.
Does doctorpatient stability affect the provision of good medical care?
Joachim P. Sturmberg
Department of General Practice, Monash University, Melbourne, Victoria, Australia
Correspondence: Joachim P. Sturmberg, Associate Professor of General Practice, PO Box 3010, Wamberal, New South Wales 2260, Australia.
Accepted for publication September 19, 2006.
Abstract
Aim: To find out whether greater doctorpatient stability is associated with better provision of good medical care.
Methods: Retrospective in-depth analysis of a random sample of patient records attending a typical four-doctor group practice in New South Wales, Australia.
Results: Recording of smoking status and alcohol consumption, blood pressure measurement, influenza vaccination, diet assessment, and discussion of chronic and psychosocial health problems were more likely to occur in those with a stable doctorpatient relationship, but tetanus vaccination in adults was less likely.
Conclusions: This study adds that doctorpatient stability per se creates an environment that positively influences the doctorpatient relationship as is evidenced by the greater likelihood of performing activities that contribute to good medical care.
Key words: consultation process, continuity of care, doctor-patient stability, quality of care
Methods: Retrospective in-depth analysis of a random sample of patient records attending a typical four-doctor group practice in New South Wales, Australia.
Results: Recording of smoking status and alcohol consumption, blood pressure measurement, influenza vaccination, diet assessment, and discussion of chronic and psychosocial health problems were more likely to occur in those with a stable doctorpatient relationship, but tetanus vaccination in adults was less likely.
Conclusions: This study adds that doctorpatient stability per se creates an environment that positively influences the doctorpatient relationship as is evidenced by the greater likelihood of performing activities that contribute to good medical care.
Key words: consultation process, continuity of care, doctor-patient stability, quality of care
Introduction
Continuity of care is considered to be a defining characteristic of family practice and implies a longitudinal relationship between patients and those who care for them. This relationship is regarded as a therapeutic one that ideally transcends multiple illness episodes and includes responsibility for preventive care and care coordination.1,2 These descriptions of continuity of care involve two different but related concepts one being longitudinal stability of the doctorpatient relationship, the other being the resulting care process, which by implication is believed to result in better health outcomes.
This paper examines the relationship between these two notions and it is hypothesized that a stable doctorpatient relationship improves the care process as documented in patient records, a proxy indicator for better health outcomes.
Method
The study was conducted in a four-doctor suburban practice on the New South Wales Central Coast, Australia. The practice is long-established (> 50 years) and the current doctors have been working there for between 5 and 22 years. The estimated practice size was 4000, with the doctors providing about 22 000 consultations per year. Power calculation determined that a sample size of 200 patients would have a reasonable chance of detecting differences in the consultation process at the 0.05 level between those with and without doctorpatient stability. Four hundred patient records were randomly selected on the assumption that only one-half of all patients would satisfy the inclusion criteria of having had at least four consultations, that is, had a minimal opportunity to engage with a preferred provider, during the study period July 1995 to June 1997. The final study population was representative of the practice population and closely matched Australian population characteristics and their utilization pattern.3,4
Doctorpatient stability was measured using three established indices: usual provider continuity (UPC the most commonly seen doctor); sequential provider continuity (SECON seeing the same provider on consecutive visits); and modified continuity index (MCI describes the density of visits with the most commonly seen provider) as it has been argued that the type of continuity measure may influence correlations.1 The footnote to Table 1 describes how each measure is calculated. Patients who had an arbitrarily chosen value of = 0.66 (i.e., 2/3 of all visits to the same/most commonly seen provider) on either scale were defined as having a stable doctorpatient relationship.
All consultation records were analyzed for evidence of a set of history, consultation activity and management items that had been identified during an academic panel discussion as indicators of good medical care. A test-retest approach of a random 10% sample of records analyzed demonstrated intra rater reliability of the data extraction process.
Data were analyzed using log-likelihood tests to compare the relationship of doctorpatient stability with the probability of the various consultation activities being conducted. The study was approved by the Ethics Committee of Monash University, Melbourne, Australia.
Results
The final sample comprised 254 patients (131 males, 123 females) and was larger than anticipated, representing about 6.4% of the total practice population. The mean age of the study population was 42.7 years (95% CI: 39.645.8; range: 095), a total of 3107 consultations were analyzed, and the mean consultation rate for males was 10.7 (95% CI: 9.611.8) and for females 13.2 (95% CI: 11.714.6) over the 2-year study period.
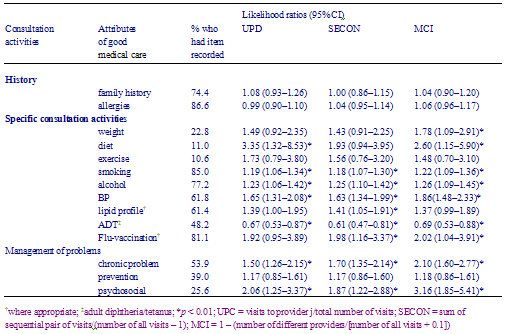
Overall a greater likelihood of specific consultation benefits was found for those with a stable doctorpatient relationship regardless of the stability measure used (Table 1). On all three measures, a stable relationship correlated with increased likelihood of measurements of smoking status, alcohol consumption and blood pressure being recorded, and of chronic and psychosocial health problems being discussed. Increased likelihood of diet advice being given and influenza vaccination being performed were found with two of the stability measures. No differences were seen in relation to the recording of family histories and allergies, and the discussion of preventive health activities. Tetanus vaccination in adults was the only activity less likely to be performed for those with a stable doctorpatient relationship.
Discussion
An ongoing doctorpatient relationship is a prerequisite, but not the essence of continuity of care. Previous studies have provided indirect evidence about the benefits of an ongoing doctorpatient relationship in the general practice setting.59 This in-depth analysis of consultations as evidenced in the patient record was conducted in retrospect without doctors or patients behavior having been influenced by the study. It adds that the consultation process differs subtly depending on patients degree of doctorpatient stability. A stable doctorpatient relationship not only leads to the accumulation of knowledge, and probable understanding about the patient,6 but also appears to change the sense of responsibility toward the patient10 as expressed by a more complete approach to patient care.
Personal provider continuity leads to tangible benefits for patient care, especially for those with chronic and psychosocial health problems, and these benefits are present regardless of the type of continuity measure used.1
The findings arise from a representative analysis of patient records in a single practice population, thus they do not allow generalization. However, the strength of this study lies in its in-depth analysis of the recorded consulting behavior of all consultations over a 2-year period with patients with and without a stable doctorpatient relationship.
Conclusion
This study adds that doctorpatient stability per se creates an environment that positively influences the doctorpatient relationship as is evidenced by the greater likelihood of performing activities that contribute to good medical care.
Acknowledgments
The statistical advice given by John Hinchy, statistician, is greatly acknowledged.
References
1 Saultz J. Defining and measuring interpersonal continuity of care. Ann Fam Med 2003; 1: 13443.
2 Haggerty J, Reid R, Freeman G, Starfield B, Adair C, McKendry R. Continuity of care: a multidisciplinary review. Br Med J 2003; 327: 121921.
3 Sturmberg J. Comprehensiveness of Care in a Small Group Practice and its Relationship to Patient Utilisation Patterns. Melbourne: Monash University, 1998.
4 Bridges-Webb C. Assessing health status in general practice. Med J Aust 1992; 157: 3235.
5 Hjortdahl P, Borchgrevink C. Continuity of care influence of general practitioners knowledge about their patients on use of resources in consultations. Br Med J 1991; 303: 11814.
6 Hjortdahl P. Continuity of care. General practitioners knowledge about, and sense of responsibility toward their patients. Fam Pract 1992; 9: 38.
7 Hjortdahl P. The influence of general practitioners knowledge about their patients on the clinical decision-making process. Scand J Prim Health Care 1992; 10: 2904.
8 Ettlinger P, Freeman G. General Practice Compliance Study: Is it worth being a personal doctor? Br Med J 1981; 282: 11924.
9 Freeman G, Richards S. Personal continuity and the care of patients with epilepsy in general practice. Br J Gen Pract 1994; 44: 3959.
10 Banahan B, Banahan BI. Continuity as an Attitudinal Contract. J Fam Pract 1981; 12: 7678.
Table 1 - Contingency table: Likelihood ratios (95% CIs) of having a particular consultation activity recorded for those with a stable doctorpatient relationship
^top