Asia Pacific Journal of Family Medicine Volume 5 Issue 2
ORIGINAL ARTICLE
Opportunities in primary care for reducing stroke rates:
a cross-sectional study of the differences in the control of hypertension between ethnic groups
Nisreen ALWAN and Chris J. PACKHAM
School of Community Health Sciences, Division of Epidemiology & Public Health, Nottingham University Medical School, Nottingham, UK
Correspondence: Dr Nisreen Alwan, 39 Plantation Avenue, Leeds LS17 8TB, UK
Accepted for publication 10 July 2006.
Opportunities in primary care for reducing stroke rates:
a cross-sectional study of the differences in the control of hypertension between ethnic groups
Nisreen ALWAN and Chris J. PACKHAM
School of Community Health Sciences, Division of Epidemiology & Public Health, Nottingham University Medical School, Nottingham, UK
Correspondence: Dr Nisreen Alwan, 39 Plantation Avenue, Leeds LS17 8TB, UK
Accepted for publication 10 July 2006.
Abstract
Aim: To compare blood pressure control and management patterns among hypertensive patients of Caucasian and ethnic minority origin.
Methods: This study involved a retrospective case-note assessment of the quality of care received over a 3-year period of 199 Caucasian and 50 ethnic minority patients with established essential hypertension attending an inner city UK general medical practice.
Results: Compared to Caucasian patients, patients from ethnic minority origins were more likely to have a mean diastolic blood pressure above 90 mmHg adjusted for age, gender, diabetes, body mass index, smoking, alcohol, and family history of cardiovascular and cerebrovascular disease (OR = 2.6, p = 0.02). Ethnic minority patients had an average of five more general practice visits annually than Caucasian patients (p < 0.01). However, the mean number of blood pressure readings per year did not differ significantly between the two groups. The most commonly used antihypertensive drug in ethnic minority patients was atenolol compared to bendroflauzide in Caucasian patients.
Conclusions: There is scope for improving the control of blood pressure, and hence influencing vascular disease rates, in ethnic minority populations. The use of evidence-based hypertension treatment tailored to ethnic origin could be improved and the higher number of GP visits for these patients could be utilized to optimize blood pressure control. However, public health strategies need to take account of the possible higher primary care workload inherent in achieving good control in such populations.
Key words: ethnicity, hypertension, primary care.
Methods: This study involved a retrospective case-note assessment of the quality of care received over a 3-year period of 199 Caucasian and 50 ethnic minority patients with established essential hypertension attending an inner city UK general medical practice.
Results: Compared to Caucasian patients, patients from ethnic minority origins were more likely to have a mean diastolic blood pressure above 90 mmHg adjusted for age, gender, diabetes, body mass index, smoking, alcohol, and family history of cardiovascular and cerebrovascular disease (OR = 2.6, p = 0.02). Ethnic minority patients had an average of five more general practice visits annually than Caucasian patients (p < 0.01). However, the mean number of blood pressure readings per year did not differ significantly between the two groups. The most commonly used antihypertensive drug in ethnic minority patients was atenolol compared to bendroflauzide in Caucasian patients.
Conclusions: There is scope for improving the control of blood pressure, and hence influencing vascular disease rates, in ethnic minority populations. The use of evidence-based hypertension treatment tailored to ethnic origin could be improved and the higher number of GP visits for these patients could be utilized to optimize blood pressure control. However, public health strategies need to take account of the possible higher primary care workload inherent in achieving good control in such populations.
Key words: ethnicity, hypertension, primary care.
Introduction
Stroke is the third most common cause of death in the UK, responsible for about 60 000 deaths a year in England and Wales.1 The public health target for the UK is to reduce the death rate from coronary heart disease and stroke in people under the age of 75 years by at least two-fifths by 2010, saving up to 200 000 lives in total.2 One major strategy for stroke prevention is the control of hypertension. A 5 mmHg reduction in diastolic blood pressure and a 9 mmHg reduction in systolic blood pressure can reduce the risk of stroke by one-third.3
Ethnic minorities form 9% of the population in England.4 There is evidence that age-standardized median systolic blood pressure is significantly higher in Afro-Caribbeans than Europeans, and mortality from hypertensive disease is four times greater among Afro-Caribbean men and seven times greater among Afro-Caribbean women than the national average. The mortality rate from stroke among Afro-Caribbeans in England and Wales is nearly twice that of the general population.57 The mortality rate related to hypertension among British Asians is about 1.5 times the national rate.8
Scarce data is available on the quality of care given to hypertensive patients from ethnic minority groups because of the challenge of routine and complete identification of ethnic origin in National Health Scheme (NHS) records. This study explores blood pressure control levels and the pattern of hypertension management among patients of different ethnic origins in a UK inner city general practice.
Materials and methods
The practice is situated in an inner city, highly deprived, area of Nottingham in England, with a 30% ethnic minority practice population. On registration, patients complete a card that includes the identification of their ethnic origin, with categories based on the England census classification. Patients were selected for the study on the basis of computer-recorded Read codes (the recommended national standard coding system in general practice in the UK for recording clinical information) with diagnosis of hypertension, and drug prescriptions for antihypertensive medications.
Data was collected from the medical records of hypertensive patients attending the practice over a 3-year period (calendar years 199698). The demographic data extracted from the medical records included ethnic group, gender and age. Clinical data collected included date of diagnosis; blood pressure level at the start of treatment; number of blood pressure readings before the initiation of medication; annual number of GP and practice nurse consultations; cardiovascular risk factors including smoking, alcohol consumption, body mass index, family history of hypertension, cardiovascular or cerebrovascular disease or diabetes mellitus; investigation results and frequency; the annual number and values of blood pressure readings; non-pharmacological treatment advice; concurrent diseases and problems; current drug treatment; and the number of hospital admissions. Manual and computer (Egton Medical Information Systems, UK) records were reviewed.
Due to differences in the target blood pressure between guidelines that were current at the time of the study,911 analysis was performed twice considering the definition of control to be 160/90 mmHg and 140/90 mmHg. In addition to the systolic and diastolic blood pressure, the mean arterial pressure (MAP) was used in the analysis (MAP = systolic pressure + [diastolic pressure * 2]/3).12
The doses of the antihypertensive drugs were expressed as fractions of the 1999 WHO Defined Daily Doses (DDDs).13 For each year of the 3-year period reviewed the total number and type of antihypertensive medication prescribed was recorded. An antihypertensive agent was included if it was taken at any time that year. Drugs were classified as per the British National Formulary.14
Sample size and power calculation
From the results of the studies performed to assess the adequacy of hypertension control in Britain, it was expected that 50% of Caucasian patients would have inadequate blood pressure control. The numbers of Caucasian and ethnic minority patients with essential hypertension in the practice gave the study an 80% power to detect an odds ratio for ethnic minority patients to have inadequate blood pressure control of 2.5 (equivalent to a level of inadequate control of 70%) at 5% (2-tailed) level of significance.
Statistical analysis
Statistical analysis was done using SPSS V.8 for Windows. Logistic regression analysis was carried out to determine which variables contributed to observed blood pressure; all variables were entered using the forward method with ethnic group entered as block two. Linear regression was used to explore the relationship between workload (number of GP and nurse visits) and other variables. Other tests, including chi-squared, t-test and MannWhitney U-test, were used as necessary to test univariate relationships. In all cases, a 2-tailed probability of less than 0.05 was taken as significant.
Results
Two hundred and forty-nine patients were identified; 199 Caucasians and 50 belonging to ethnic minority groups. These included 39 Black and 11 South Asian patients. Basic demographic and risk factor differences are displayed in Table 1.
Seventy-four patients (30%) were tested at least once during the 3-year period for total serum cholesterol (61 Caucasian and 13 ethnic minority patients), and about 20% of both groups had a 3-year average serum cholesterol of over 6.5 mmol/L with no significant difference between the two groups. There were no significant differences in the number of urine, serum glucose or electrolyte tests, non-pharmacological lifestyle advice, number of drugs used between ethnic minority groups and drug doses taken, calculated as fractions of DDDs, between Caucasian and ethnic minority patients over the study period (Table 2). However, the most commonly prescribed antihypertensive drug in ethnic minority patients was atenolol compared to bendrofluazide in Caucasians.
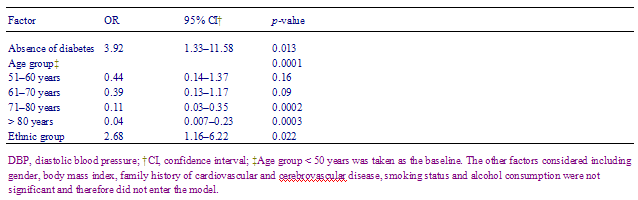
The average number of blood pressure measurements prior to initiation of pharmacological treatment was three times for both groups. The average blood pressure at the initiation of treatment was 175/102 for Caucasian and 168/102 for ethnic minority patients (ρ = 0.036). The mean DBP for ethnic minority patients was 90 mmHg, compared to 87 mmHg for Caucasian patients. Of ethnic minority patients, 55% had a diastolic blood pressure over 90 mmHg during the 3-year study period, compared to 33% of Caucasian patients (χ2 = 7.83, df = 1, ρ = 0.005) (Table 3). The difference remains significant following adjustment for eight potential confounding factors using the logistic regression model (p = 0.02) (Table 4). The odds ratio of ethnic minority patients having a DBP more than 90 mmHg was 2.7 (95% CI 1.26.2).
The mean systolic blood pressure for the 3-year period of the study was 157 mmHg for all hypertensive patients in the practice (158 mmHg for whites and 152 for ethnic minority patients). The difference at either threshold was not significant between the two ethnic groups. The odds ratios of having SBP more than 160 mmHg for patients aged 6170, 7180 and more than 80 years were 5, 8.1, 11.5, respectively. At the lower 140 mmHg threshold for SBP control, in addition to age, female hypertensives were 3.5 times more likely to have SBP higher than 140 mmHg than male hypertensives (95% CI 1.48.7, ρ = 0.006).
The only factor that had a significant effect on whether the mean arterial pressure (MAP) was below or above the control threshold was the body mass index of the patient. The odds ratio for a patient with a body mass index of more than 27 kg/m2 of having a MAP more than 113.3 mmHg (160/90 mmHg) was 2.7 (95% CI 1.45.3).
The mean number of GP and nurse visits per year for ethnic minority patients was 7.1 and 1.0, respectively. For Caucasian patients, the number of visits was 5.8 and 1.3, respectively. Adjusting for age and sex using linear regression, ethnic group had a significant independent effect on measured workload (OR = 4.4, 95% CI 0.38.5, p = 0.035) including both nurse and doctor visits with the difference in the number of visits to the GP alone greater (OR = 4.8, 95% CI 1.38.3, p = 0.008). There was no significant difference in the annual number of blood pressure readings following the diagnosis of hypertension (3 for Caucasians and 4 for ethnic minority patients).
Diabetic patients had significantly higher rates of practice consultations, including both nurse and GP visits with a mean difference of eight visits (95% CI 412).
Discussion
People with hypertension from ethnic minorities from the study population were about two and a half times more likely to have inadequate control of their diastolic blood pressure (defined as more than 90 mmHg), despite having a higher overall GP consultation rate than Caucasian patients. There was no significant difference in the number of blood pressure readings between the two groups.
Only 47% of ethnic minority patients had their average DBP controlled (less than 90 mmHg) compared to 77% of Caucasian patients, a finding that was still significant after extensive adjustment for important clinical differences between the groups. The proportion of hypertensives not receiving drug treatment in our population was lower than shown in other studies (12% of Caucasians and 14% of ethnic minorities), and the level of control achieved was higher, suggesting that either the threshold for drug treatment in our population was lower or that fewer difficult-to-control patients presented to the primary care team.15
Previous studies have failed to demonstrate consistent findings in blood pressure levels by ethnicity. Most of the UK studies performed in this field had limited covariate adjustment,5,6,16,17 that is, usually adjusting for two or three factors only, while in this study we adjusted for eight. All eight factors taken into account can act as potential confounders of the relationship examined.
Although the overall GP workload was higher for ethnic minority patients in this setting, the number of consultations in which blood pressure was measured between Caucasian and ethnic minority patients was similar with an interval between blood pressure measurements of about 3 months in both groups, in line with current recommendations.18
One striking finding in this study was that non-diabetics were more likely to have inadequately controlled DBP. One explanation is that diabetics visited the practice more frequently and that their hypertension was treated more assiduously. Another possible explanation is that antidiabetic non-pharmacological measures taken by these patients worked in favor of their blood pressure control.
Study limitations
The studys strength lies in that most of the factors that can affect the relationship between ethnicity and blood pressure control have been adjusted for in the analysis. However, the study has several limitations. Due to the limited size of the study population we combined patients from different ethnic minority backgrounds in one group to achieve the required statistical power. The justification for this is that, although the two ethnic minority groups (Black and South Asian) differ in many characteristics, they share the increased cardiovascular risk compared to the Caucasian population. Another limitation was that we did not differentiate between recently diagnosed hypertensive patients and those who were diagnosed many years ago who may have been better controlled.
Recommendations
The findings of this study suggest that, despite the fact that hypertensive patients from ethnic minority populations have a higher average number of annual GP visits than the Caucasian population, additional interventional activity may be necessary if better outcomes in hypertension control are desired. One such intervention could be increasing the number of blood pressure measurements for ethnic minority patients. Another would be using evidence-based medicine to determine the choice of antihypertensive medications prescribed. In this study, atenolol was the most commonly prescribed antihypertensive in ethnic minority patients, who were mainly of African descent in our population. Recent evidence suggests that β-blockers tend to be less effective than other alternatives at lowering blood pressure in Black patients especially if used as monotherapy.19
More intensive management of hypertensive patients from ethnic minority origin in primary care has potential resource implications. Whether the higher number of practice visits made by ethnic minority people could be better utilized for this purpose needs to be investigated. Further work is required to assess the cultural implications of the management of hypertension in ethnic minority patients, and possible subsequent effects on primary care workload.
Acknowledgments
The authors would like to thank the practice staff and patients of St Lukes Surgery, Radford, Nottingham and Dr Jim Pearson, Division of Epidemiology and Public Health, Nottingham University, for helpful advice on the statistical analyses.
References
1 Director of Public Health/Nottingham Health district. The Annual report 1998: Mens Health. Nottingham: Nottingham Health Authority, 1998.
2 Department of Health. Saving Lives: Our Healthier Nation. Available at: http://www.ohn.gov.uk (Accessed 19 February 2004.)
3 Swales JD. Manual of Hypertension. Oxford: Blackwell Science,1995.
4 Census 2001. Available at: http://www.statistics.gov.uk (Accessed 19 February 2004.)
5 Haines AP, Booroff A, Goldberg E, Morgan P, Singh M, Wallace P. Blood pressure, smoking, obesity and alcohol consumption in black and white patients in general practice. Journal of Human Hypertension 1987; 1: 3946.
6 Chaturverdi N, McKeigue PM, Marmot MG. Resting and ambulatory blood pressure differences in Afro-Caribbeans and Europeans. Hypertension 1993; 22: 906.
7 Health Education Authority (HEA). Hypertension and the African-Caribbean community. Guidance for Health Professionals. London: Health Education Authority, 1998.
8 Raleigh VS. Diabetes and hypertension in Britains ethnic minorities: Implications for the future of renal services. British Medical Journal 1997; 314: 20913.
9 World Health Organisation-International Society of Hypertension. 1999 Guidelines for management of hypertension.. Journal of Hypertension 1999; 17: 15185.
10 . Coope J. Hypertension. London: Royal College of General Practitioners, 1993.
11 Sever P, Beevers G, Bulpitt C, et al. Management guidelines in essential hypertension: Report of the Second Working Party of the British Hypertension Society. British Medical Journal 1993; 306: 9837.
12 Dillon A, Lyon J, Coombs MA. Haemodynamic Profiles and the Critically Ill Patient: a Practical Guide. Oxford: BIOS Scientific Publishers, 1997.
13 World Health Organisation Collaborating Centre for Drug Statistics Methodology. ATC index with DDDs 1999. Oslo: World Health Organisation, 1999.
14 British Medical Association-Royal Pharmaceutical Society of Great Britain. British National Formulary (number 35). London: British Medical Association-Royal Pharmaceutical Society of Great Britain, 1998.
15 Colhoun HM, Dong W, Poulter NR. Blood pressure screening, management and control in England: results from the Health Survey for England 1994. Journal of Hypertension 1998; 16: 74752.
16 Cappuccio FP, Cook DG, Atkinson RW, Strazzullo P. Prevalence, detection, and management of cardiovascular risk factors in different ethnic groups in south London. Heart 1997; 78: 55563.
17 Cruickshank JK, Jackson SH, Beevers DG, Bannan LT, Beevers M, Stewart VL. Similarity of blood pressure in blacks, whites and Asians in England: the Birmingham Factory Study. Journal of Hypertension 1985; 3: 36571.
18 World Health Organization. WHO Technical Report Series 862. Hypertension Control. Geneva: World Health Organization, 1996.
19 Gibbs C, Beevers D, Lip G. The management of hypertensive disease in Black patients. Quarterly Journal of Medicine 1999; 92: 18792.
Table 1 - Demographics, cardiovascular risk factors and blood pressure control. Indicators for the study population using univariate analysis
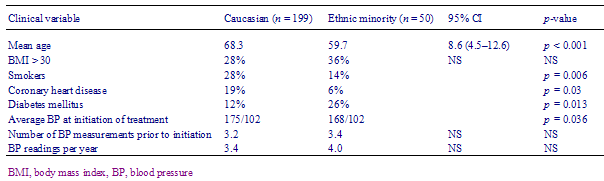
Table 2 - Number of antihypertensive drugs prescribed for Caucasian and ethnic minority patients in one study year
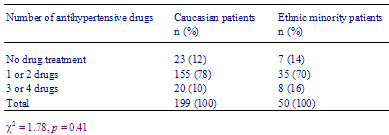
Table 3 - Percentage of Caucasian and ethnic minority patients with uncontrolled average MAP, SBP and DBP during the study period using univariate analysis
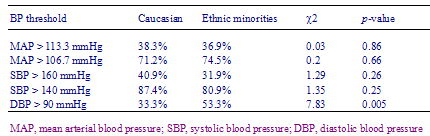
Table 4 - The effect of ethnicity on the control of DBP (taken as < 90 mmHg) adjusted for the significant factors entered in the logistic regression model (forward method)