
Asia Pacific Journal of Family Medicine Volume 5 Issue 2
ORIGINAL ARTICLE
Future career in general practice specialty?
Will undergraduate course experience make any difference?
Siew Beng KHOO
Department of Family Medicine, Penang Medical College, Penang, Malaysia,
No. 4 Sepoy Lines Road, Penang 10450, Malaysia.
Accepted for publication 16 August 2006.
Future career in general practice specialty?
Will undergraduate course experience make any difference?
Siew Beng KHOO
Department of Family Medicine, Penang Medical College, Penang, Malaysia,
No. 4 Sepoy Lines Road, Penang 10450, Malaysia.
Accepted for publication 16 August 2006.
Abstract
Background: A community-based general practice course has been developed in the Penang Medical College (PMC) (a joint Ireland-Malaysia venture) that simultaneously satisfies the medical regulatory authorities in Ireland and re-orients the current medical education to the health needs of the Malaysian community.
Objectives: This paper describes the community-based general practice course in PMC, explores student evaluation of the various course objectives, student perception of general practice in Malaysia, and whether course experience has any influence on their choice of general practice specialty as a future career.
Methods: Two consecutive classes of students (n = 78) were invited to complete anonymous, confidential pre-general practice rotation and post-general practice rotation course questionnaires.
Results: Overall responses from both classes were 75/78 (96.1%) for pre-course and 73/78 (93.6%) for post-course questionnaire. Although students had minimal knowledge of Irish and Malaysian primary health care before the course, 60% were keen to learn about Irish primary healthcare and 54.7% expected to learn about the Malaysian healthcare system in the course. Overall, there was a slight reduction of No response and increment of Maybe response after the course with regard to working as a general practitioner in both countries but statistical tests show that there is no significance in the difference.
Conclusions: An innovative community-based general practice course has been implemented in PMC but course experience of students does not seem to have any influence on their choice of general practice specialty as a future career.
Key words: community, general practice course, Ireland, Malaysia, primary healthcare.
Objectives: This paper describes the community-based general practice course in PMC, explores student evaluation of the various course objectives, student perception of general practice in Malaysia, and whether course experience has any influence on their choice of general practice specialty as a future career.
Methods: Two consecutive classes of students (n = 78) were invited to complete anonymous, confidential pre-general practice rotation and post-general practice rotation course questionnaires.
Results: Overall responses from both classes were 75/78 (96.1%) for pre-course and 73/78 (93.6%) for post-course questionnaire. Although students had minimal knowledge of Irish and Malaysian primary health care before the course, 60% were keen to learn about Irish primary healthcare and 54.7% expected to learn about the Malaysian healthcare system in the course. Overall, there was a slight reduction of No response and increment of Maybe response after the course with regard to working as a general practitioner in both countries but statistical tests show that there is no significance in the difference.
Conclusions: An innovative community-based general practice course has been implemented in PMC but course experience of students does not seem to have any influence on their choice of general practice specialty as a future career.
Key words: community, general practice course, Ireland, Malaysia, primary healthcare.
Introduction
This paper describes the community-based general practice course in the Penang Medical College (PMC), explores student perceptions of general practice in Malaysia, and whether the course has any influence on their choice of general practice specialty as a future career.
Primary healthcare in Malaysia
Malaysia has a dual system of healthcare delivery that exist side-by-side and are independent of each other. Government sector health services are concerned with curative, rehabilitative, promotive, preventive and regulatory measures, while the private sector is urban-based and predominantly curative.1
Primary healthcare in the public sector is provided by the outpatient/casualty departments of general hospitals and community health clinics. In the private sector, it is provided by general practitioners (GPs), specialists in private hospitals, specialists with open access clinics and other health care providers such as dentists, pharmacists, alternative medicine therapists, Chinese and Malay traditional and spiritual healers.
A Malaysian GP who has completed the 3-year compulsory service in the public health sector can set up a private practice without the requirement of vocational training or postgraduate examination. Consultations and dispensing of drugs are carried out in general practice clinics; patients are self-paying and not registered with any particular general practice.
General practice course in Penang Medical College
Penang Medical College (PMC) is a private college. It is a joint IrelandMalaysia venture in which students spend their initial 2½ pre-clinical years in either UCD (University College Dublin) or RCSI (Royal College of Surgeons) and the remaining 2½ years of clinical training in PMC. PMC took its first intake of students in 1996 and the first cohort graduated in 2001. This paper describes the feedback from students of two consecutive classes, (4th intake [n = 39] and 5th intake [n = 39]) where for the first time, the general practice course was amalgamated into a continuous 8-week block in rotation with paediatrics/obstetrics and gynecology/psychiatry (POPGP program) at the beginning of the final medical year.
For this 8-week general practice course, students are exposed to the public and private health sectors that provide different types of services, ranging from primary prevention and health promotion, to therapeutic, rehabilitative and palliative care for the terminally ill. Students gain valuable experience from clinical attachments and home visits at the community clinics, helping them to understand the health problems of the under-privileged population in rural areas. Private general practice tutors provide students with the opportunity to understand the roles of GPs in Malaysia, the problems involved in running a private practice and a view of the spectrum of acute, chronic and undifferentiated illnesses in the community. Geriatric care is taught in a charitable community home for the aged; students interactions with the elderly residents helps them to develop an optimistic and positive attitude and to understand the concept of independence, productivity and dignity of the elderly. Home visits with the Hospice Home Program nurses helps them appreciate the complexities of medical, social, psychological, cultural and spiritual problems faced by patients with advanced malignancy. Direct contact with children and their parents during their visits to the spastic childrens center helps them to appreciate the experiences of people with disabilities in our community and the long-term difficulties faced by their carers.
Classroom teaching includes tutorials, case presentations, dermatology slide shows, clinical skills workshops and introductory lectures on sports and occupational medicine. Communication skills videotaping and analysis improves their consultation skills and teaches them how to handle bad news and difficult questions.
In the Personal and Family Health project students are required to follow-up a case from hospital to community and vice versa over a period of 6 weeks. Emphasis here is on the impact of illness on the equilibrium of family dynamics, psychosocial and environmental factors involved, and the strengths and weaknesses of our primary healthcare system. This learning model allows them to progress through a learning pathway of exploration within community settings driven by the acts of listening to and reflecting on the lives of their patients. Students interests in alternative/complementary medicine is reflected in the informal Hot Topics sessions, as many of them chose to talk about Tai-chi, Qigong, moxibustion, aromatherapy, acupuncture, hypnotherapy and spiritual healing.
Methods
A pre-general practice course questionnaire was developed to assess students knowledge of Irish and Malaysian primary healthcare, their personal opinion of general practice in Malaysia, their expectations of what they may achieve from this general practice course and whether they consider taking up general practice as a future career. A post-general practice course questionnaire assessed changes in their personal opinion of general practice in Malaysia after attending the course, whether their expectations were met and whether there was any change in their consideration of taking up general practice as a future career. Various course objectives were evaluated using a Likert scale of 1 (implies very little, useless) to 10 (implies a lot, useful). Neither questionnaire was piloted before the study.
Students of the 4th (n = 39) and 5th intakes (n = 39) were invited to complete the anonymous, confidential pre-course questionnaire on the first day of the general practice course and to complete the post-course questionnaire at the end of it.
Application for ethics approval was not required for this study.
Participants subjective comments about the course were summarized using themes and quantitative data was analyzed with the Medcalc program .
Results
Overall, responses from both classes were 75/78 (96.1%) for the pre-course questionnaire and 73/78 (93.6%) for the post-course questionnaire. Table 1 shows the demographic details of the two classes of students, demonstrating that the majority were Chinese, that the peak student age was 2325 years, and that the ratio of male to female students was roughly equal.
In the pre-course questionnaire students demonstrated a minimal knowledge of both the Malaysian and the Irish healthcare system; about 60% could not offer one correct statement with regard to the features of both healthcare systems; 60% were keen to learn about Irish healthcare. In addition, they were asked to list three good and three bad points regarding Malaysian general practice from their personal perspective. These responses were grouped into favorable and unfavorable opinions (Table 2). While about eight students regarded a lower academic requirement as favorable, an equal number regarded it as unfavorable.
Comparison of results before and after the GP course
Of particular note is the changes in personal opinions that have occurred before and after taking the general practice course:
- Better understanding of Malaysian primary healthcare and role of GPs in the community (see Table 3).
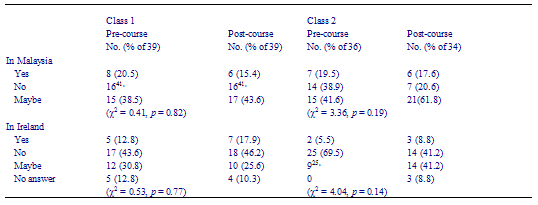
- Better understanding of the similarities and differences between Irish and Malaysian primary healthcare, although the course appeared to make no significant difference as to whether the student was considering being a GP in either Ireland or Malaysia (see Table 4).
- Change of perception of general practice from playing an unimportant role, of dealing mainly with coughs and colds, to an important role with vast amounts of responsibility, skill and knowledge.
- Higher regards for general practice.
- Realization of the importance of geriatric and palliative care in our community.
- Appreciation of the importance of holistic approach to patient care, of communication skills and of learning something completely different from what is taught in hospitals.
Discussion
The World Health Organization points out that the burden of disease and health needs vary from country to country. Clinical conditions that are important in a developed country may be less important in a less well resourced one. Teaching therefore needs to be sensitive to this and to be balanced with knowledge of the major health issues relevant to the developing country.2 A significant innovation in the educational bridges between Ireland and Malaysia is to satisfy the medical regulatory authorities in Ireland and to re-orient current medical education to respond toward the health needs of the community in Malaysia3 The vast differences between Irish and Malaysian primary health care, while posing great challenges, provides an opportunity to create a unique general practice program.
Students came to us with minimal knowledge of the features of both Irish and Malaysian primary health care, but the majority expressed an interest to know more about both systems and expected to learn about Malaysian health care and the role of GPs in the community. Our aim in this course is not to recruit or train future GPs but rather, if all students, including those who are going to be future hospital specialists, have a better understanding of how primary care functions, much will have been achieved.4 In particular, as moral attitude focuses on the capacity to respond to others in a humane manner, incorporating palliative care into medical training has been shown to not only improve the quality of palliative care but also contribute to the moral aspects of attitude,5
About 45% of students were still undecided in their final medical year about which specialty they would like to pursue, 20.5% were considering general practice as a career in Malaysia, while 12.8% were considering this in Ireland. This course allowed students to be better informed by providing a better understanding of Irish and Malaysian primary health care, the role of GPs in the community, and cultivating higher regard and respect for general practice.
It has been shown that students experiences in medical school, particularly during clerkships, have significant impact on their specialty choice, and that medical schools wishing to increase the number of their graduates entering family practice should strongly consider clinical rotations in family medicine and providing maximum exposure to faculty members as role models.6 However, in spite of positive responses, the only change in answer was the overall decreased response for No and increased response for Maybe after the course for class 2, with regard to working as a GP in Ireland or Malaysia. Chi-square testing showed that this difference is not significant. This may be due to a different cohort of students with different personal perspectives on general practice. More important factors that contribute to their choices may be: the structure of general practice in individual countries; prospect of career development; nature of the job; status; income; family commitment; decision to serve ones own country; or the challenges and experience of working in a foreign country with a different culture. With vast differences in the culture, community resources and health care needs of both countries, is it possible to equate the PMC general practice course to that of UCD, RCSI or an international standard? Cohen acknowledged the need to preserve local characteristics of curricula. As he puts it: a common set of international standards does not imply equivalence of educational content nor graduates, educational objectives and the means by which they are attained will vary.7 Staff from both Ireland and Malaysia must also need to understand and to learn from and about the health care models of each others country.4
Conclusion
The general practice course in PMC has developed and implemented a model of learning that draws upon a wide range of community resources. Students have the advantage of understanding two different models of health care that will be valuable to them whether they are going to work in Malaysia or in Ireland. However, in spite of positive responses from students, their general practice course experience in PMC did not seem to influence their choice of general practice specialty as a future career in these two cohorts of students.
Acknowledgments
Special thanks to Professor Gerard Bury of UCD, Dublin, for his contribution in setting up this GP Course and Professor Tom Hennessy, Founder Dean of PMC, for his support of our program. We deeply appreciate the support from the public health authorities, part-time lecturers, private general practice tutors, staff of Physiotherapy/Occupational Therapy Units of Penang General Hospital, staff of community health clinics, residents of the Home for the Aged of the Little Sisters of the Poor, nurse coordinators of Hospice Home Programme, staff of Spastic Childrens Association of Penang and last but not least the contributions from all the community patients and their families in sharing their experiences with us.
References
1 Chee HL. Health and health care in Malaysia. Available at: http://www2.jaring.my/pcdom/monotoc.htm.
2 Bundred P, Gibbs T. Facing up to the realities of global medical education in the 21st century. Medical Education 2002; 36: 600.
3 Malaysian Medical Association. Reorientation of Medical Education for the Primary Health Care. Tan Sri Datuk Dr Abdul Khalid bin Sahan. Available at: http://www.mma.org.my/info/1_phc_87.htm
4 Bury G, Cullen W, Khoo SB. Educational bridges between Ireland and Malaysia: Initial student responses to the Penang Medical College project. Asia Pacific Family Medicine 2003; 2: 2005.
5 Olthuis G, Dekkers W. Medical education, palliative care and moral attitude: some objectives and future perspectives Medical Education 2003; 37: 928.
6 Brearly WD, Simpson W, Baker RM. Family practice as a specialty choice: effect of premedical and medical education. Journal of Medical Education 1982; 57: 44954.
7 Ole Ten C. Global standards in medical education what are the objectives? Medical Education 2002; 36: 602.
8 General Medical Council. Tomorrows doctors. Recommendations on undergraduate medical education. 1993; London: General Medical Council. Available at: http://www.gmc-uk.org/med_ed/tom-doc.htm.
Table 1 Student demographic data
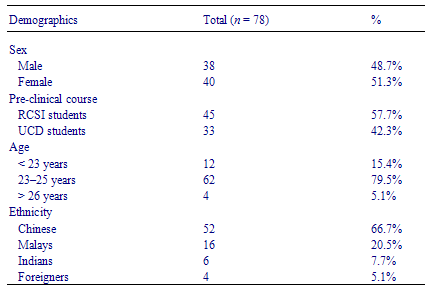
Table 2 Personal opinion of general practice in Malaysia
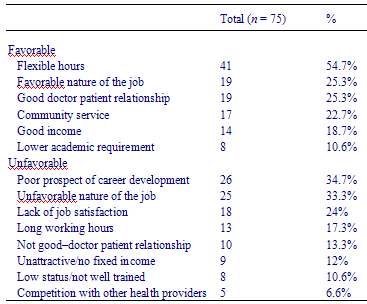
Table 3 Expectations from the PMC general practice course

Table 4 Would you consider being a GP in Ireland/in Malaysia? (n = 75)


^top