
What Keeps them Going? The Story of A Family Dealing with Stroke
Lillian FAUSTINO LAO, Melody DUMANHUG, Maria Elinore ALBA-CONCHA and Rex CARBONILLA
Department of Family and Community Medicine, Davao Medical Center, Davao City, Philippines
George Santayana
Introduction
Stroke is the second leading cause of death globally.1 This disease has also continued to rise in the Philippines. Stroke leaves patients debilitated, the consequence of which is functional impairment that results in ongoing suffering for the patient and the family As physicians, we bear witness to the physical discomfort caused by the disease as well as the emotional, social and economic consequences it causes. This makes us ask ourselves: How do patients and families cope?
This article uses a family health case history model to present some of the issues raised by this disease from a patient-centred approach and how their medical care is integrated into this.
Mr KH, a 72-year-old, Japanese man was diagnosed with hypertension in 1986. He was also noted to be an alcoholic. He was a non-smoker. His blood pressure was controlled with perindopril 4 mg once daily, averaging 130/80, but with a BP range of 130/80180/120.
He was apparently well until December 13, 2002 when he noted numbness of both feet, which he ignored. The following day, he was found unconscious on the floor of his home. He was admitted to ICU, at a nearby hospital where he remained for a month, requiring mechanical ventilation until a tracheostomy tube was inserted.
Due to financial constraints, he was transferred to a government facility The initial diagnosis was that of cerebrovascular accident (CVA), right temporal lobe non-hemorrhagic infarct, lacunar infarct, left centrum semiovale; aspiration and nosocomial pneumonia; hypertensive ischemic cardiovascular disease (CVD); and ischemic cardiomyopathy.
Physical examination on transfer revealed a stuporous patient with stable vital signs. Neurology-wise, extraocular muscle movements (EOMs) were full, there was no nystagmus, no facial assymetry but with absent gag reflex, weakness on all extremities, more prominent on the left, with incontinence and best verbal response was with eye-opening.
Snapshot of the family
KHs family is a small, inter-racial, unilaterally extended and non-hierarchical. Looking at the genogram in Fig. 1, we see that our patient, a Japanese divorcee, remarried Cory, a 42-year old Filipina and they had a son Yoshi, who was 13 years old at the time of the stroke. Corys niece, Daisy, 16 years old, was also living with them. Not much is known about KHs family except that his father was also a divorcee and that he lived with his father and stepmother. Cory on the other hand is the third in a sibling-set of seven. The hereditary/familial illnesses present in the families are also highlighted in the genogram. Prior to the illness, KH was the familys sole breadwinner and decision-maker, while Cory was the main caregiver. After the stroke, Cory had to assume both roles.
Impact of illness in a family
According to Carter and McGoldrick, KHs family is at the life-cycle stage of a family with adolescents.6 This stage is said to be the crisis stage for the family since the couple has to contend with both renegotiating relationships as well as the demands of a teenage son. Despite this, they were relatively content and happy prior to the onset of the illness. The family experienced its first major setback with Sedgewick Corporation closing down and KH being forced to retire in 1998. At first, he was not worried because he was certain his pension would cover their expenses. However, because of the delay in its release, this put pressure on the family finances and he became withdrawn from his family. Cory was not very helpful at this stage because she partly put the blame on her husbands unemployment as the cause of the tighter budget for the family. This event was followed in 2002 by KHs CVA that left him debilitated, hence draining the familys resources further.
Addressing disease within a family framework
So what resources were available to the family at the time of the illness that could help or hinder them in dealing with the illness? The Social Cultural Religion Economic Education Medical (SCREEM) tool in Table 1 highlights the familys resources and weaknesses. We can see that generally the family has adequate intrafamilial and extrafamilial resources to help them deal with the illness. The major burden lies in being able to handle finances well.
Despite the familys resources and good relations prior to the illness, when they first came in contact with the Family Health Care Program (FHCP), the family APGAR (Adaptation, Partnership, Growth, Affection, Resolve; this assessment tool was originally designed by Smilkstein to assess family function and is a rapid screening instrument for the family dysfunction and has adequate reliability and validity to measure an individuals level of satisfaction about family relationships), was severely dysfunctional. This was brought about by the sudden changes in roles, the increasing demands on Cory to be the decision-maker, breadwinner and caregiver, while simultaneously losing communication with KH. The family map across the different family life events is illustrated in Fig. 2. We see the marked deterioration in family relations from the time when KH was working, after his retirement and after he became ill. We see that he withdrew from his family after his retirement, and when he became sick, communication between family members declined further, each becoming preoccupied with their own distress.
Medical issues and interventions
At the time of referral to the FHCP team, complications brought about by the stroke such as pneumonia, decreased mobility, incontinence and contractures were urgent concerns. Apart from that, the hypertension that led to the stroke needed to be addressed.
Hypertension was controlled with an ACE inhibitor. Initially, KH was started on Citicholine for stroke. A meta-analysis by Davalos et al. revealed that oral Citicholine at a dose range of 5002000 mg given within the first 24 h in patients with moderate to severe stroke increased the chances of complete recovery at 3 months.2 However, in another randomized controlled trial, where Citicholine 1000 mg was given twice daily for 6 weeks, no significant difference in outcome measures was noted between those given the drug and those given placebo.3 These conflicting findings and the fact that there was no improvement after 2 months of treatment and the additional cost that the therapy was posing for the family, made the FHCP team decide to discontinue the drug.
Pneumonia was resolved with antibiotic treatment. Tracheostomy care, chest physiotherapy to mobilize secretions was also advised. Long-term goals included weaning from the tracheostomy tube. Decreased mobility, incontinence and contractures were dealt with by educating the caregivers on prevention of these complications. Instructions on how to bathe, feed, position and do passive range of motion exercises were also given. Another medical issue raised was the probability of rehabilitation. Aggressive rehabilitation was not pursued further since KHs National Institutes of Health Stroke Scale (NIHSS) score for stroke severity indicated that this was severe. Patients with severe stroke are poor candidates for aggressive rehabilitation since they have poor prognosis for functional recovery.4
Psychosocial issues and interventions
Psychosocial issues based on the familys psychosocial profile included the communication barrier brought about by the disease, the possible depression of Cory, the toll of the disease on Yoshi, caregiver fatigue and the financial burden of the illness.
Here, one-on-one counselling was done with Cory to ventilate her fears and address her concerns. She was also affirmed in her role of decision-maker for the family now that KH was unable to do so. Support for their young son was also given as he adjusted to the illness. The stressful life events they had to undergo, starting with KHs termination from work, followed by his illness, initially put the family out of equilibrium. However, with available resources, such as: a Japanese association network; the identification of medical and psychosocial issues and timely interventions from the FHCP team; intrafamilial resources; and the ability of the family to accept, grow and reorganize from the loss, the family has coped and adapted well, thus establishing a new equilibrium.
It is from this point that they continue to move on with the knowledge that whatever the future may bring, they have each other from which to draw strength.
References
1 Anonymous. Asia Pacific Consensus Forum on Stroke Management. Stroke 1998; 29: 17306.
2 Davalos A, Castillo J, Alvarez-Sabin J, et al. Oral citicoline in acute ischemic stroke: an individual patient data pooling analysis of clinical trials. Stroke 2002; 33: 28507.
3 Clark WM, Wechsler LR, Sabounjian LA, Schwiderski UE, Citicoline Stroke Study Group. A phase III randomized efficacy trial of. mg citicoline in acute ischemic stroke patients. Neurology 2000; 57: 1595602.
4 Veterans Health Administration. VA/DoD clinical practice guideline for the management of stroke rehabilitation in the primary care setting. Washington (DC): US Department of Veteran Affairs, 2003.
5 Smilkstein G. The cycle of family function. A conceptual model for family medicine. Journal of Family Practice, 1980; 11: 22332.
6. Carter EA, McGoldrick, M. The Family Life Cycle: A Framework for Family Therapy. New York: Gardner, 1980.
Table 1 Social Cultural Religion Economic Education Medical (SCREEM) tool
|
Resources |
Pathology |
Social |
Networks with Japanese association |
Lack of communication with his family in Japan |
|
Harmonious relationship with school community |
|
|
Harmonious relationship with wife and son |
|
Cultural |
Strong ties with Japanese community hence the family |
|
|
got support from them |
|
Religion |
No religious differences in dealing with the sick |
No family unity in religious activities since |
|
|
Cory is Catholic and Kenshee is Buddhist |
Economic |
Presence of savings |
Expensive medical care |
|
Assets and collectibles |
Cory not empowered to make financial decisions prior to |
|
Income from rented house |
Kenshee’s illness |
|
Pension at around Php 40 000 every 2 months |
|
Education |
Cory has the ability to comprehend medical instructions |
Perceived lack of caregiving skills |
|
|
and advice |
Medical |
Prompt response to basic medical needs |
Cory easily persuaded to buy instruments that people say |
|
with basic home equipments |
Kenshee needs |
Figure 1 Himura-Basco family genogram
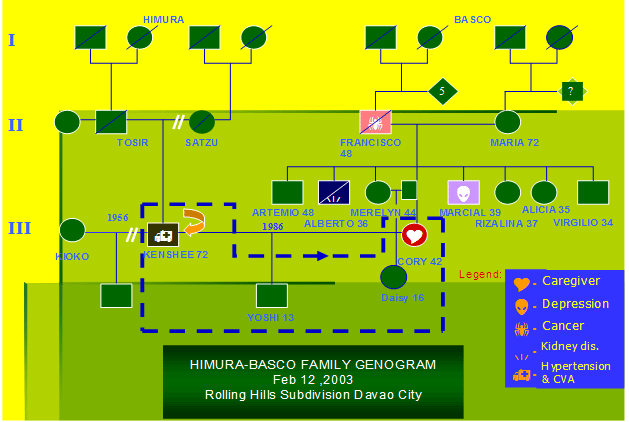
Figure 2 Family map across different life events
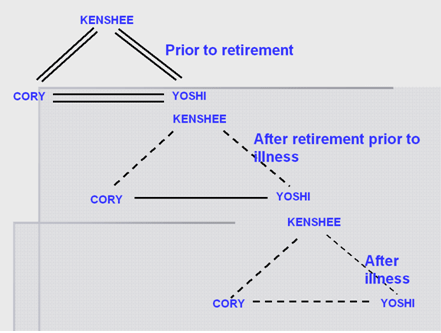
Figure 3 Smilksteins Cycle of Family Function
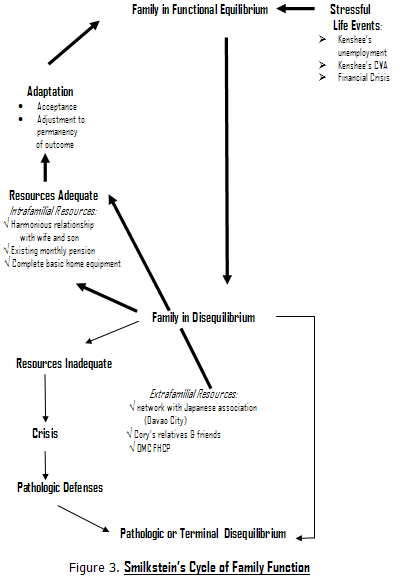
^top