
Asia Pacific Journal of Family Medicine Volume 5 Issue 1
ORIGINAL ARTICLE
Hyperlipidaemia: a pilot of a multidisciplinary intervention in general practice
Parker MAGIN, Dimity POND, Surinder BAINES and Susan GOODE
University of Newcastle, Newcastle, New South Wales, Australia
AbstractHyperlipidaemia: a pilot of a multidisciplinary intervention in general practice
Parker MAGIN, Dimity POND, Surinder BAINES and Susan GOODE
University of Newcastle, Newcastle, New South Wales, Australia
Background and aim: Hyperlipidaemia is a major health concern, and general practitioners have a pivotal role in its management. This pilot study aimed to deliver an efficacious, truly multidisciplinary, hyperlipidaemia management package involving optimal genreal practice medical care together with dietician and nurse educator input.
Methods: Subjects identified as having elevated cholesterol levels in a previous study together with their general practitioners (GPs) were recruited. The subjects received an intervention comprising dietician assessment and advice; and nurse-delivered exercise education. Their GPs participated in a workshop on hyperlipidaemia management and cardiovascular risk stratification. The acceptability of the intervention was assessed. Other outcome measures were serum cholesterol, other cardiovascular risk factors and dietary parameters, as well as GP knowledge and practice.
Result: The intervention was acceptable to subjects. There were significant reductions in serum cholesterol levels and cigarette consumption. There was a non-significant trend for subjects to be doing more moderate-level or vigorous exercise. There were no changes in blood pressure, BMI or waist-to-hip ratio. There were favorable changes, though mainly non-significant, in dietary intake.
Conclusions: The results of this pilot study were encouraging and the intervention is suitable for further study.
Key words: anticholesteremic agents, cholesterol, diet, exercise, family practice
Methods: Subjects identified as having elevated cholesterol levels in a previous study together with their general practitioners (GPs) were recruited. The subjects received an intervention comprising dietician assessment and advice; and nurse-delivered exercise education. Their GPs participated in a workshop on hyperlipidaemia management and cardiovascular risk stratification. The acceptability of the intervention was assessed. Other outcome measures were serum cholesterol, other cardiovascular risk factors and dietary parameters, as well as GP knowledge and practice.
Result: The intervention was acceptable to subjects. There were significant reductions in serum cholesterol levels and cigarette consumption. There was a non-significant trend for subjects to be doing more moderate-level or vigorous exercise. There were no changes in blood pressure, BMI or waist-to-hip ratio. There were favorable changes, though mainly non-significant, in dietary intake.
Conclusions: The results of this pilot study were encouraging and the intervention is suitable for further study.
Key words: anticholesteremic agents, cholesterol, diet, exercise, family practice
Introduction
Hyperlipidaemia is established as a major health concern due to strong causal relationships with ischaemic heart disease1 ischaemic stroke2 overall mortality1 and due to its high prevalence.3 There is also strong evidence of the efficacy of cholesterol-lowering in reducing morbidity and mortality4,5 related to hyperlipidaemia.
Both pharmacological and non-pharmacological approaches have been evaluated in hyperlipidaemia management. Pharmacotherapy has been shown to reduce total cholesterol levels and to reduce cardiovascular mortality and morbidity, in both patients with6 and without a history of ischaemic heart disease,7 and to reduce stroke morbidity and mortality.8 There are currently consensus guidelines for the use of lipid-lowering drugs, but there are also suggestions that a large number of patients who would benefit from lipid-lowering therapy do not receive it9 or do not achieve recommended targets.10 Studies suggest that general practitioner (GP) knowledge and the implementation of cardiovascular risk stratification11 and hyperlipidaemia management guidelines12 may be poor. In addition, identifiable barriers to guideline implementation result in wide variations in patterns of statin prescribing.13
Diet is generally regarded to be the cornerstone of hyperlipidaemia management and has been shown to produce reductions in cholesterol levels (though by modest amounts and limited by compliance)14 and in cardiovascular and overall mortality.15 Furthermore, exercise has been shown to reduce cholesterol levels and to delay the progression of atherosclerotic coronary heart disease.16
It may be thought that a multidisciplinary approach that addresses these three issues of medication, diet and exercise would be optimal, and that general practice would be the ideal environment for delivery of such a multidisciplinary approach.
In general practice, nurse-led cardiovascular individual,17 family18 and group19 lifestyle interventions; nurse-delivered brief health behavior20 and exercise21 interventions, and pharmacist-initiated interventions,22 have produced variable results in lifestyle change. Their applicability to reductions in cholesterol levels and coronary risk scores and implications for change in general practice have been debated.2330 Dietician telephone coaching has resulted in lowering of lipid levels.31
The introduction of care-planning items into the Australian Medicare benefits schedule (whereby GPs could be remunerated for coordinating the care of patients by multiple health professionals) presented an opportunity to deliver a more efficacious, truly multidisciplinary, hyperlipidaemia management involving optimal GP medical care together with dietician and nurse educator input. This article presents the results from an optimal general practice-based multidisciplinary intervention incorporating diet and exercise components within a GP care-planning framework. The study hypothesis was that such an intervention would produce favorable changes in serum cholesterol levels and in other cardiovascular risk factors. A major objective of the study was to assess the feasibility of delivery and acceptability to patients of the intervention.
Method
The intervention was planned as a pilot study for a subsequent randomised controlled trial.
Subjects identified as having elevated serum cholesterol levels (> 5.5 mmol/L or > 212 mg/dL) in the Broken Hill Proprietry (BHP) Health and Unemployment Study of blue-collar workers retrenched in the Newcastle BHP steelworks closure of 199932 were invited to participate. A serum cholesterol level > 5.5 mmol/L was chosen as 5.5 mmol/L was the upper limit of serum cholesterol recommended by the National Heart Foundation of Australia33 for cardiovascular health in the general population. Following agreement to participate, participants GPs were also invited to be part of the study. Both patient and GP were required to consent to participation for entry into the study.
All subjects received the intervention. There was no control group.
Subjects visited their GPs who assessed their suitability for the project and any contraindications to the exercise component of the study and completed a brief questionnaire on the subjects medical history and medications. If the GP felt the patient met the criteria for a co-ordinated care plan it was completed at this stage, listing the study dietician and nurse as other care givers.
Subjects were visited by a study nurse (at a place convenient to the subject in most cases the subjects home) who performed baseline measures of height, waist-to-hip ratio, blood pressure and cholesterol (using Accutrend GC). The subjects dietary intake was assessed using a food-frequency questionnaire (Dietary Questionnaire for Epidemiological Studies, Version 2. Melbourne: The Cancer Council Victoria, 1996). Subjects self-completed a baseline questionnaire consisting of questions relating to demographics, smoking, alcohol use, medications, exercise, family history, diagnoses and treatment of hyperlipidaemia, and history of hypertension, diabetes, peripheral vascular disease and heart disease. Four months following the intervention the subjects baseline measures and dietary questionnaire were repeated.
The intervention comprised three components:
1 An individual education session on healthy physical activity/exercise delivered by a nurse. The study recommendations were based on the physical activity guidelines of Australias National Heart Foundation (NHF) and were supported by pamphlets produced by the NHF. The 30-minute physical activity session included the benefits of exercise (in particular the benefits for people with elevated cholesterol) and the level and duration of exercise necessary to achieve health benefits, individualized according to the subjects interests and physical capabilities.
2 An individualized dietary consultation conducted by a dietitian. The half-hour dietary sessions were designed to promote healthy eating advice with particular emphasis on modifications to current dietary practices as determined by each participants eating habits and information from the dietary questionnaires. All participants were given printed resources (NHF patient education leaflets) regarding healthy eating practices with emphasis on reducing fat consumption (particularly saturated fat), and increasing dietary fiber and decreasing consumption of refined carbohydrates. The leaflets also covered issues of healthy weight maintainance, decreased salt intake, moderation of alcohol intake, and smoking cessation.
3 A 2-hour workshop for participating GPs on cardiovascular risk assessment and implementation of hyperlipidaemia consensus guidelines in general practice.
General practitioners knowledge and practice of hyperlipidaemia management were surveyed using a self-administered questionnaire before and 3 months after the workshop. Patient acceptability of the intervention was determined by self-completed questionnaire after completion of the study.
Outcome measures were:
1 Changes in subject serum cholesterol levels, blood pressure, body mass index, waist-to-hip ratio, exercise levels, and dietary parameters.
2 Changes in levels of hypolipidaemic medication prescription.
3 Changes in GP knowledge and practice regarding hyperlipidaemia management.
4 Acceptability of the multidisciplinary management package to subjects including subject opinions of the usefulness, relevance, and behavioral impact of the intervention.
Statistical analysis was performed using the Statistical Package for the Social Sciences (SPSS). Analysis of continuous data was undertaken using paired t-tests or Wilcoxon signed rank test. Categorical data were analysed with McNemars test or binomial distribution.
Ethics approval for the study was obtained from the University of Newcastle Human Research Ethics Committee.
Results
Sixty-two subjects from the BHP Health and Unemployment Study were identified as having had serum cholesterol levels > 5.5 mmol/L. Fifty-seven potential participants were able to be contacted and invited to participate in the study. Thirty-four subjects agreed to participate but only those subjects whose corresponding GP agreed to participate were entered into the study. Of the 21 subjects who were entered into the study, 20 completed all elements of the intervention and post-intervention assessments.
Demographics
Demographic characteristics of the sample are summarized in Table 1.
Acceptability
There was a low drop-out rate. Twenty of the 21 subjects completed all elements of the program. The usefulness and relevance of the intervention were highly rated by subjects and the behavioral impact was positively rated (see Tables 2 and 3). All subjects agreed that the intervention was beneficial. Forty percent of subjects agreed that the program had positively affected their GPs management of the subjects cholesterol. Five percent disagreed with the statement that the intervention had positively affected their GPs care of them. Fifty-five percent of the subjects reported a neutral response to this statement.
Changes in cardiovascular parameters and lifestyle, dietary and exercise behaviors
Cardiovascular-risk factors, lifestyle, dietary and exercise changes results are summarized in Tables 48.
There were statistically significant reductions in serum cholesterol levels (0.5 mmol/L, 95% CI 0.140.86), number of cigarettes smoked per day, and the number of subjects drinking on five or more days per week. Following the intervention significantly more subjects reported considering health effects when making dietary choices. There were no changes in rates of hypolipidaemic prescription.
There was a non-significant trend for subjects to be undertaking more moderate-level or vigorous exercise. There were no changes in blood pressure, BMI or waist-to-hip ratio.
Carbohydrate intake significantly increased. There was a statistically significant reduction in polyunsaturated fat intake and non-significant trends to less total fat, saturated fat and cholesterol and to increased fiber.
GPs knowledge and practice of hyperlipidaemia management
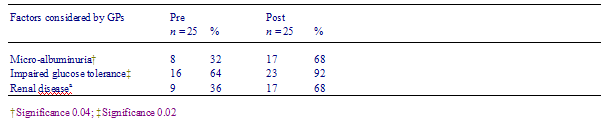
There were no changes in hypolipidaemic medication prescription. At a 3 months post-education session there were significant changes in GPs consideration of three of 19 clinically relevant factors in hyperlipidaemia risk stratification (see Table 9).
Discussion
This pilot study demonstrated the feasibility of delivery and the acceptability to patients of a multidisciplinary management package for hyperlipidaemia.
The simple before-and-after design of this pilot project, with no control group, along with the use of total cholesterol rather than a complete lipid profile as an outcome measure, renders any conclusions based on these results limited, but the results are never-the-less worthy of comment.
Although the intervention was of limited numbers and power, a significant reduction in serum total cholesterol levels was achieved. This is also noteworthy in view of the recruitment methodology which resulted in some of the subjects having already been identified as being hyperlipidaemic by their GPs prior to the start of the study (and having had management including pharmacotherapy in one case already commenced). The mean reduction in cholesterol levels was clinically as well as statistically significant. The mean decrease in total cholesterol levels was 0.5 mmol/L. A reduction of serum cholesterol of 0.6 mmol/L sustained for 5 years has been estimated to result in a reduction of incidence of ischaemic heart disease of 50% at age 40, falling to 20% at age 70.4 A reduction of total cholesterol of 9% as achieved in this study would be expected to reduce coronary heart disease mortality by 13%.5
The lack of change in hypolipidaemic prescription in the study suggests that positive effects on cholesterol were likely due to the targeted diet and exercise components of the therapeutic package. In this context it should be noted that in a previous randomised controlled trial34 clinician-delivered advice regarding diet, exercise and smoking had failed to lower lipid levels (although pharmacotherapy did), and in a further trial35 patients who received a dietician-delivered intervention achieved greater cholesterol lowering than did patients who received dietary advice only from their physician. In a further study, a follow-up visit to a GP by subjects found to be hyperlipidaemic at workplace screening was found not to significantly decrease cholesterol levels or improve lifestyle risk behaviors.36 A conclusion from these results and considerations would be that the multidisciplinary diet and exercise program employed in this study appears to be an appropriate means of implementing a cholesterol-lowering strategy in general practice.
While report bias was possible in this uncontrolled study, the non-significant trend to more moderate-intensity and vigorous exercise is of interest particularly as in the nurse-delivered exercise intervention it was stressed that exercise was a life-time commitment, and so had to be enjoyable for the subject (to promote long-term compliance). The nurse discussed and negotiated an exercise regimen that was practicable and acceptable to the patient. It might have been expected that an increase in lower-intensity and moderate-intensity exercise was a more likely outcome than an increase in vigorous exercise.
The reductions in the number of cigarettes smoked per day and in the number of subjects drinking on five or more days per week were also of interest as these were not specific targets of the intervention (though they were mentioned in the supporting literature provided to patients). The authors would propose that these changes may have been related to the subjects having become, post-intervention, more health-oriented or health-focused.
The nutritional intervention promoting healthy eating practices with particular emphasis on reducing intake of dietary fat, particularly saturated fat, and increasing consumption of fiber resulted in favorable trends in dietary changes. There was a trend for participants to increase their intake of dietary fiber and for the total fat consumption to be reduced, as was the intake of saturated fat. Though not all of the dietary changes were statistically significant, taken together with the participant evaluations of dietary impact of the intervention, it seems that nutritional counselling by a dietitian may have enabled the participants to modify their dietary practices to be more in line with healthy eating recommendations.
There was relatively little change in GPs knowledge and practice post-intervention. To a large degree this could be seen to be attributable not just to the limited power of this pilot study to detect changes but also to the baseline knowledge, and adherence to current lipid-management guidelines, of this group of GPs already being good. The significant increases in GPs consideration of microalbuminuria, renal disease and impaired glucose tolerance in vascular risk stratification was encouraging.
The generalisability of this result, in blue-collar male subjects, to the wider hyperlipidaemic population could be questioned. However, there is little in the protocol that is likely to be less acceptable to a wider patient population. Given that men are at higher cardiovascular risk than women37 and that lower socio-economic class is associated with higher cardiovascular risk (and may even be an independent risk factor for cardiovascular disease)38,39 it might be thought that acceptability of the intervention to this group is particularly relevant to interventions targeted at a wide range of sociodemographic groups.
Criticism has been directed at the cost-effectiveness of general practice-based cardiovascular risk factor interventions.25,26,30,40 Largely for this reason there is a strong argument for concentrating efforts at lipid-lowering to secondary prevention and to primary prevention in patients at high cardiovascular risk (with consideration of lipid levels as only one factor in overall risk stratification).4144 Since this study was carried out, there have been changes in the requirements for care plan-based remuneration in Australia, and it is quite likely that criteria for funding of this type of intervention may be reviewed and may change in the future. Similarly, organizational and remuneration structures in other countries may vary widely. The delivery of the intervention trialled in this study would need to be adapted to local and current health organization structures. For example, in Australia at present, this intervention could be provided to patients with diabetes or existing cardiovascular disease within current care planning arrangements (and would thus be consistent with the argument for directing lipid-lowering strategies at high-risk groups).
Conclusion
The multidisciplinary team approach to hyperlipidaemia management employed in this pilot study has been found to be practicable, acceptable and likely to result in improved patient outcomes. The authors are currently planning a randomised controlled trial in a population of higher cardiovascular-risk hyperlipidaemic patients in general practice, with longer follow-up, to further evaluate the efficacy (and sustainability of the effects) of this intervention.
Acknowledgments
The study was supported with a Royal Australian College of General Practitioners/Australian Association of Academic General Practitioners Cardiovascular Research Grants in General Practice grant.
Summary of implications for GPs
Hyperlipidaemia is a major health problem in the community. The great majority of hyperlipidaemia is managed in general practice. Diet, exercise and hypolipidaemic medications have all been shown individually to reduce cholesterol. A combined approach incorporating all three elements would seem optimal. General practice is the natural setting for the delivery of such a combined intervention. This study suggests a multidisciplinary general practice-centred intervention is practicable and worthy of further evaluation.
References
1 Martin MJ, Hulley SB, Browner WS, Kuller LH, Wentworth D. Serum cholesterol, blood pressure, and mortality: implications from a cohort of 361,662 men. Lancet 1986; 2: 9336.
2 Anonymous. Blood pressure, cholesterol, and stroke in eastern Asia. Eastern Stroke and Coronary Heart Disease Collaborative Research Group. Lancet 1998; 352: 18017.
3 Sempos CT, Cleeman JI, Carroll MD et al. Prevalence of high blood cholesterol among US adults. An update based on guidelines from the second report of the National Cholesterol Education Program Adult Treatment Panel. JAMA 1993; 269: 300914.
4 Law MR, Wald NJ, Thompson SG. By how much and how quickly does reduction in serum cholesterol concentration lower risk of ischaemic heart disease? BMJ 1994; 308: 36772.
5 Gould AL, Rossouw JE, Santanello NC, Heyse JF, Furberg CD. Cholesterol reduction yields clinical benefit. A new look at old data. Circulation 1995; 91: 227482.
6 Randomised trial of cholesterol lowering in 4444 patients with coronary heart disease: the Scandinavian Simvaststin Survival Study (4S). Lancet 1994; 344: 13839.
7 Downs JR, Clearfield M, Weis S et al. Primary prevention of acute coronary events with lovastatin in men and women with average cholesterol levels: results of AFCAPS/TexCAPS. Air Force/Texas Coronary Atherosclerosis Prevention Study. JAMA 1998; 279: 161522.
8 Hebert PR, Gaziano JM, Chan KS, Hennekens CH. Cholesterol lowering with statin drugs, risk of stroke, and total mortality. An overview of randomized trials. JAMA 1997; 278: 31321.
9 Holt N, Johnson A, de Belder M. Patient empowerment in secondary prevention of coronary heart disease. [Comment]. Lancet 2000; 356: 314.
10 Vale MJ, Jelinek MV, Best JD, Health CsgCpoAC. How many patients with coronary heart disease are not achieving their risk-factor targets? Experience in Victoria 199698 versus 19992000. Medical Journal of Australia 2002; 176: 2115.
11 McManus RJ, Mant J, Meulendijks CF et al. Comparison of estimates and calculations of risk of coronary heart disease by doctors and nurses using different calculation tools in general practice: cross sectional study. BMJ 2002; 324: 45964.
12 Frolkis JP, Zyzanski SJ, Schwartz JM, Suhan PS. Physician noncompliance with the 1993 National Cholesterol Education Program (NCEP-ATPII) guidelines. Circulation 1998; 98: 8515.
13 Fairhurst K, Huby G. From trial data to practical knowledge: qualitative study of how general practitioners have accessed and used evidence about statin drugs in their management of hypercholesterolaemia. BMJ 1998; 317: 11304.
14 Yu, -Poth S, Zhao G, Etherton T, Naglak M, Jonnalagadda S, Kris-Etherton PM. Effects of the National Cholesterol Education Programs Step I and Step II dietary intervention programs on cardiovascular disease risk factors: a meta-analysis. American Journal of Clinical Nutrition 1999; 69: 63246.
15 Hooper L, Summerbell CD, Higgins JP et al. Dietary fat intake and prevention of cardiovascular disease: systematic review. BMJ 2001; 322: 75763.
16 Franklin BA, Kahn JK. Delayed progression or regression of coronary atherosclerosis with intensive risk factor modification. Effects of Diet, Drugs, and Exercise. Sports Medicine 1996; 22: 30620.
17 Cupples ME, McKnight A. Five year follow up of patients at high cardiovascular risk who took part in randomised controlled trial of health promotion. BMJ 1999; 319: 6878.
18 Wood D, Kinmonth A, Davies G et al. Randomised controlled trial evaluating cardiovascular screening and intervention in general practice: principal results of British family heart study. BMJ 1994; 308: 31320.
19 Lindholm LH, Ekbom T, Dash C, Eriksson M, Tibblin G, Schersten B. The impact of health care advice given in primary care on cardiovascular risk. CELL Study Group. BMJ 1995; 310: 11059.
20 Steptoe A, Doherty S, Rink E, Kerry S, Kendrick T, Hilton S. Behavioural counselling in general practice for the promotion of healthy behaviour among adults at increased risk of coronary heart disease: randomised trial. BMJ 1999; 319: 9437; discussion 9478.
21 Naylor PJ, Simmonds G, Riddoch C, Velleman G, Turton P. Comparison of stage-matched and unmatched interventions to promote exercise behaviour in the primary care setting. Health Education Research 1999; 14: 65366.
22 Tsuyuki RT, Johnson JA, Teo KK, Simpson SH, Ackman ML, Biggs RS et al. A randomized trial of the effect of community pharmacist intervention on cholesterol risk management: the Study of Cardiovascular Risk Intervention by Pharmacists (SCRIP). Archives of Internal Medicine 2002; 162: 114955.
23 Hobbs FD. Study was grossly underpowered (letter). BMJ 2000; 321: 49.
24 Smith GD, Ebrahim S, Bennett R. Non-attendance for follow-up distorts results and shows that people dont like counselling. BMJ 2000; 321: 49.
25 Haq IU, Jackson PR, Yeo WW, Ramsay LE. Interventions in OXCHECK study waste resources. BMJ 1995; 311: 260.
26 Wonderling D, Langham S, Buxton M, Normand C, McDermott C. What can be concluded from the Oxcheck and British family heart studies: commentary on cost effectiveness analyses. BMJ 1996; 312: 12748.
27 Ebrahim S, Smith GD. Systematic review of randomised controlled trials of multiple risk factor interventions for preventing coronary heart disease. BMJ 1997; 314: 166674.
28 Steptoe A, Doherty S, Kendrick T, Rink E, Hilton S. Attitudes to cardiovascular health promotion among GPs and practice nurses. Family Practice 1999; 16: 15863.
29 Moore H, Adamson AJ, Gill T, Waine C. Nutrition and the health care agenda: a primary care perspective. Family Practice 2000; 17: 197202.
30 Toop L, Richards D. Preventing cardiovascular disease in primary care. BMJ 2001; 323: 2467.
31 Vale MJ, Jelinek MV, Best JD, Santamaria JD. Coaching patients with coronary heart disease to achieve the target cholesterol. a method to bridge the gap between evidence-based medicine and the real world randomized controlled trial. Journal of Clinical Epidemiology 2002; 55: 24552.
32. Pond D, Harris E, Magin P et al. A brief intervention to manage unemployment in General Practice. Newcastle: Discipline of General Practice, University of Newcastle, 2004.
33. www.heartfoundation.com.au/statistics/docs/hsv_disease_2001 Site visited March 26, 2003.
34 Guillen M, Kornhauser C, Samaniego V, Lerdo de Tejada A. Once-daily pravaststin compared with dietry advice in patients with borderline and moderate primary hypercholesterolaemia. Current Therapeutic Research 1995; 56: 30517.
35 Henkin Y, Shai I, Zuk R et al. Dietary treatment of hypercholesterolemia: do dietitians do it better? A randomized, controlled trial. American Journal of Medicine 2000; 109: 54955.
36 Wang JS, Carson EC, Lapane KL, Eaton CB, Gans KM, Lasater TM. The effect of physician office visits on CHD risk factor modification as part of a worksite cholesterol screening program. Preventive Medicine 1999; 28: 2218.
37 Jousilahti PMD, Vartiainen EMD, Tuomilehto JMD, Puska PMD. Sex, age, cardiovascular risk factors, and coronary heart disease: a prospective follow-up study of 14 786 middle-aged men and women in Finland. Circulation 1999; 99: 116572.
38 Luepker RV, Rosamond WD, Murphy R et al. Socioeconomic status and coronary heart disease risk factor trends. The Minnesota Heart Survey. Circulation 1993; 88: 21729.
39 Kaplan GA, Keil JE. Special Report. Socioeconomic Factors and Cardiovascular Disease. A Review of the Literature. Circulation 1993; 88: 197398.
40 Langham S, Thorogood M, Normand C, Muir J, Jones L, Fowler G. Costs and cost effectiveness of health checks conducted by nurses in primary care: the Oxcheck study. BMJ 1996; 312: 12658.
41 Durrington PN, Prais H, Bhatnagar D, France M, Crowley V, Khan J et al. Indications for cholesterol-lowering medication: comparison of risk-assessment methods.[comment][erratum appears in Lancet 1999 July 10; 354 (9173): 166]. Lancet 1999; 353: 27881.
42 Grundy SM, Pasternak R, Greenland P, Smith SJ, Fuster V. Assessment of Cardiovascular Risk by Use of Multiple-Risk-Factor Assessment Equations: a Statement for Healthcare Professionals From the American Heart Association and the American College of Cardiology. Circulation 1999; 100: 148192.
43 Law MR, Wald NJ. Risk factor thresholds: their existence under scrutiny. BMJ 2002; 324: 15706.
44 Levi CR, Magin PJ, Nair BR. Primary stroke prevention: refining the high risk approach. Medical Journal of Australia 2002; 176: 3034.
Table 1 Baseline demographics and body mass index for subjects
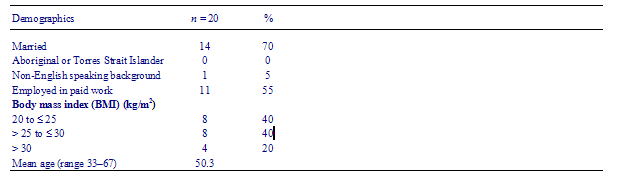
Table 2 Subject evaluation of exercise education session
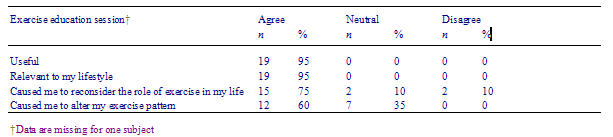
Table 3 Subject evaluation of nutrition education session
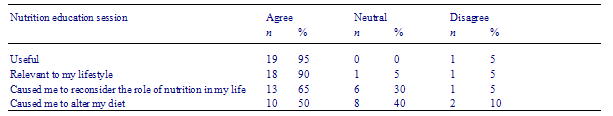
Table 4 Prepost changes in lifestyle of subjects
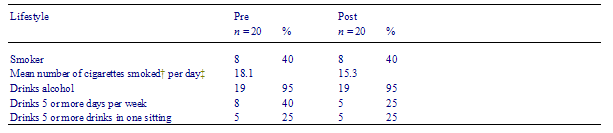
Table 5 Prepost cardiovascular related measures of subjects
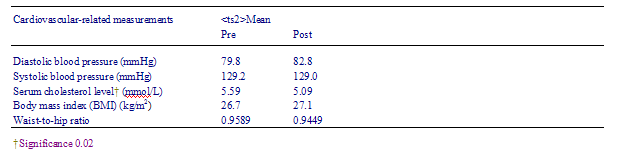
Table 6 Prepost dietary measures of subjects
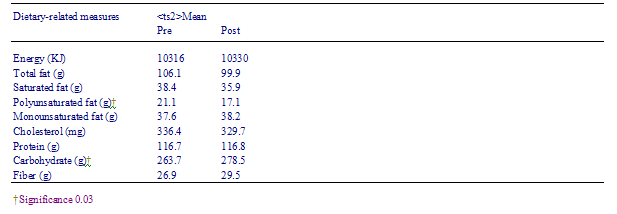
Table 7 Prepost dietary habits of subjects
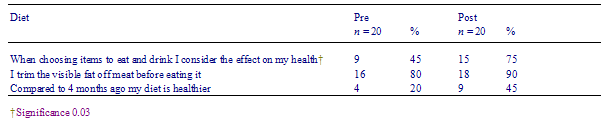
Table 8 Prepost exercise measures of subjects
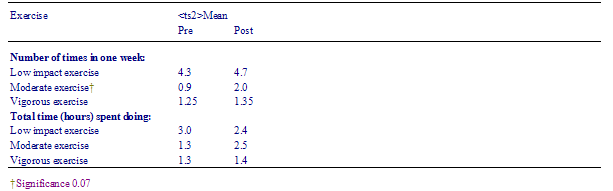
Table 9 General practitioners consideration of clinically relevant factors in hyperlipidaemia risk stratification
^top