Patient experience with self-styled family practices and conventional primary care in Thailand
Yongyuth PONGSUPAP1 and Wim VAN LERBERGHE2
1Ministry of Public Health (National Health Security Office, Nonthaburi, Thailand) and 2World Health Organization, Geneva, Switzerland
Aim: To measure level of satisfaction of patients after using services, in various domains of responsiveness (basic amenities, prompt attention, communication, dignity and trust) in 37 self-styled family practices in 16 provinces, in comparison with 37 randomly selected facilities of each of the other three types of services: public hospital outpatient departments (OPDs), private clinics and private hospital OPDs in the same provinces.
Methods: Analysis of 888 interviews with patients during an exit survey.
Result: The self-styled family practices have advantages in all domains of responsiveness when compared to public hospital OPDs. Attention was perceived to be more prompt in private clinics and private hospitals, but for the other domains, self-styled family practices provided greater patient satisfaction. Self-styled family practices and public hospitals were felt to be trusted more than private clinics and hospitals.
Conclusions: These results provide support for the policy decision to develop family practice in Thailand.
Key words: family practice, patient satisfaction, primary care, responsiveness
Introduction
The (modern) Thai health care system is essentially biomedical and hospital-centred and has been so since its introduction at the end of the nineteenth century. Both supply and demand are dominated by a reliance on technology and specialties; health care is essentially a commodity.1,2
Over the last 10 years there have been attempts to develop family practice in Thailand. This was largely a reaction against the lack of emphasis on the human dimension of health care by the system. However, family practice also addresses a number of other issues: improved responsiveness, increased patient-centredness, decreased medicalization, controlled costs and enhanced patient satisfaction. Largely an initiative of public sector doctors, the development of family practice has been seen as a way to attract patients who, traditionally, would seek to consult private practitioners.
Family practice is a relatively new concept in Thailand but has become a major issue since 2001, when the reform of the Thai health care system (also known as 30 baht scheme) assigned it a pivotal role in the organization and financing of the new system.3 Its actual origins stretch back a decade, to a group of self-styled family practitioners. These doctors had been developing a series of procedures and strategies, such as home visits for patient registration, patient follow-up, referrals to hospitals, and a rationalized information system built around family folders and teamwork.
One cannot yet speak of a fully developed professional identity. The Thai College of Family Practitioners was only created in 1999, and formal training is just starting. Nevertheless, a number of self-styled family practitioners started operating during the late 1990s, within a loose network of doctors who have attended a variety of training courses and internships. The prime movers have obtained official recognition of their family practice from the Ministry of Public Health. This paper examines patient satisfaction, using data from exit surveys, to assess whether family practice has a comparative advantage over conventional care in Thailand.
Method
We conducted exit surveys on a random sample of 888 (444 male and 444 female) patients. Six were interviewed in each of the 37 prime mover, self-styled family practices 31 based in public health centres and six based within public hospital outpatient departments (OPDs) in 16 provinces. The same survey was conducted among samples of six patients in conventional outpatient services in 37 public hospitals, 37 private clinics and 37 private hospitals in the same provinces.
The survey recorded patient information (age, education, occupation, reasons for choice of facility, symptoms/conditions for which care was sought) along with a set of questions relating to various domains of responsiveness (Table 1 and Figs 13). It also gave the opportunity for patients to suggest any improvements.
The experience with responsiveness in family practices was compared to the three other types of conventional primary care settings by subtracting the scores of the latter from the scores given to family practices. This has the advantage of being more readily interpretable than a straightforward comparison of scores, which, as expected in the Thai context where it is culturally difficult to express criticism, all cluster at the high end of the ranges. The significance of the differences in scores, was tested by MannWhitney U and Chi-square (Χ 2) tests.
Results
Of the 942 individuals approached 888, (94%) agreed to be interviewed. The majority of patients questioned fell within the 4060 years age group (male = 34%, female = 32%). Younger patients constituted a larger percentage in private clinics and hospitals than in family practices and public hospitals. Approximately half of those interviewed were employed (male = 41%, female = 37%), or farmers (male = 12%, female = 11%). There were more employees, students and businessmen among those using private hospitals and clinics, and more farmers, housewives, civil servants and the unemployed in public facilities. The majority of those interviewed had primary school education (male = 40%, female = 42%). Patients attending family practices tended to be less well educated than those attending private clinics and hospitals (Table 2).
We found no significant differences between the male and female responses, and therefore combined them in the results presented below. The most common symptom or condition for which care was sought was the same in all facilities (common cold and/or headache and/or fever). Review of chronic diseases, for example, diabetes mellitus and/or hypertension, was found to be more common in family practices (27.6%) and public hospitals (10.5%), than private hospitals (3.4%) and private clinics (2.4%).
In the majority of cases, the most frequent reason (patients could give more than one) for choosing a particular facility was proximity to the home and convenience (family practices: 80.3%; public hospitals: 61.3%; private clinics: 43.8%; and private hospitals: 50.5%). The second most frequent reason varied: for family practices, it was a short waiting time (26.9%); for public hospitals and private clinics, that they cater to older patients (22.4% and 30.4%, respectively); for private clinics another frequent reason given was the presence of specialists (24.0%); and for private hospitals the availability of good and modern technology (34.1%). In terms of the doctorpatient relationship, this was regarded as good by 12.6% of patients in family practice, a figure much higher than in the other settings: public hospitals (2.4%), private clinics (8.8%) and private hospitals (5.1%).
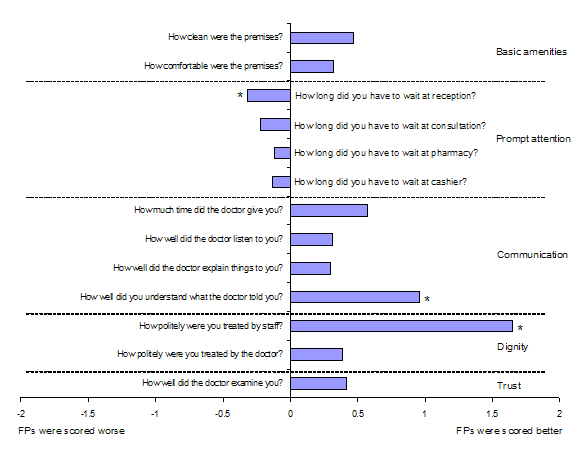
In the domains of basic amenities, communication and dignity, family practices were rated better than all the other settings; while attention was felt to be prompt in private clinics and waiting time for reception and consultation shorter in private hospitals (Figs 13). Family practice scored better on questions regarding patients trust in the doctor they consulted. Asked whether patients would choose to use this facility again, 91.5% of patients using family practices replied that they would, more than in public hospital OPDs (86.6%), private clinics (74.8%) and private hospitals (79.8%). With regards to whether the patient would recommend the doctor to friends and relatives, again, a significant proportion, as compared to the other settings, of patients consulting doctors in family practices replied that they would: family practices (93.3%); public hospital OPDs (81.5%); private clinics (77.1%); and private hospitals (74.8%).
Asked for reasons for dissatisfaction or for suggestions for improvements to services, most had no suggestions or complaints (private clinics: 76.9%, private hospitals: 75.7%, family practices: 62.3% and public hospitals: 57.8%). Only 31.5% of all those interviewed expressed one or more areas of concern. The major complaints were problems of queuing in public hospitals (17.6%), lack of technology or equipment in family practices (11.2%), and expense in private hospitals (10.7%). There were no significant complaints reported in private clinics.
Discussion
Exit surveys to measure level of patient satisfaction in the developing world has commonly found that a higher proportion of patients reported Good or Very good (in commonly used three- to five-point scales).46 In the Thai culture, doctors are traditionally held in very high regard, and thus people are particularly unwilling to criticize them.7,8 This factor is likely to be compounded by the Thai culture of consideration and respect (Kreangjai in Thai language), which inhibits open criticism of others. Combined, these factors suggest that Thai patients responding to exit surveys might be reluctant to express negative opinions about health care providers, resulting in all scores being relatively high for all categories and for all facilities. However, the instrument used in this survey proved sensitive enough to reveal some interesting, and clear, differences in patients views.
The main reason for patients to choose self-styled family practices was proximity to their home and convenience, and the majority of patients had minor illnesses (similar to conventional primary care in OPDs). Patients with chronic conditions also expressed a desire to obtain their follow-up care in self-styled family practices rather than in other facilities. This may be taken as a sign of confidence in these family practices, although normally in the public sector patients with chronic conditions would attend the hospital and are seldom dealt with in the existing Thai health centres.
Few people commented on doctorpatient relationships. This tended to be a more common factor influencing patients within self-styled family practices, but it was felt to be a minor one when compared to other issues. This may reflect the respect implicit in Thai society which needs to be taken into account in terms of general medicine within Thailand.
Patients were more explicit when commenting on whether a doctors level of specialty was a reason for choice. This was seen as a reason to consult private clinics. A facilitys perceived quality, accessibility, and equipment were reasons for visiting private hospitals. This confirms the strong biotechnical and specialist-based nature of the Thai health care system and patients expectations of their healthcare system and the component facilities.
This study goes on to show that private facilities are not the only ones willing to change and adapt (and are expected to do so) to meet their patients preferences. Self-styled family practices scored higher in terms of amenities (cleanliness and comfort) and dignity (politeness of doctors and staff). However, prompt attention (waiting times at all stations) was a problem for family practices. This may be a question of learning how to organize their services more efficiently, in respect to an appointment system and set opening hours, convenient to the patients, in order to ensure an even spread of patients during the day and between centres.
In terms of communication, the personal consultation is one of the key features, and strengths, of family medicine. Family practices consistently scored higher than other facilities, but throughout all facilities scores allocated for the question, How do you rate the way the doctor explained things to you? was significantly lower than for the question, How do you rate the way you understood what the doctor told you?. This suggests an appreciation of manner, rather than the real content, of communication. Furthermore, due to the influence of manner, it is difficult to interpret the responses to the question, How do you rate the way the doctor listened to you? which is a key element in determining quality of consultation.9 Self-styled family practices were scored higher in the categories concerning doctors time and time spent listening to patients when compared to conventional primary care. The lower score for public OPDs in this respect was predictable, given the fact that they are generally the most utilized and can be extremely crowded, and are in general need of down-sizing.
Regarding whether respondents would use the facilities again or recommend them to others, surprisingly, the public sector, including public hospitals as well as family practices, received higher scores than private clinics and hospitals. When asked for suggestions for improvements that could be made, more ideas were put forward from patients visiting self-styled family practices and public hospitals, suggesting a greater openness to debate, self-expression and the sharing of ideas, perhaps due in part, to patients feeling of ownership and familiarity with public facilities. Moreover, while conducting this survey, patients, especially in family practices, often mentioned that they were pleased that the service was being evaluated and their opinions were being considered as important. It appeared that simply involving patients and asking their opinions served as an unplanned public relations exercise.
Satisfaction with health care is closely linked to patients expectations and the degree to which they are met. A clearer understanding of these expectations may help with the interpretation of these results. However, our findings have, to a large extent, showed that the motivation of self-styled family practitioners and the user-friendly context of their practices, lead to improvements in health care provision. It is not possible to determine to what extent the various elements of training and self-study have contributed, and to what extent self-selection and motivation explain this relatively higher level of satisfaction of patients.
This study shows that doctors who wish to work as family practitioners can provide services that are rated as good as, if not better, than those of the private sector, in some categories. While we have to take into consideration that family practices are still relatively new and may still be considered new and innovative, and therefore attractive, to the populations they serve, the present findings, that self-styled family practices are generally thought to provide a better service, should be an incentive for national policy makers to give support to a new and prominent role of family practice within the health system. The next step needed is the construction of the necessary quality monitoring schemes for sustainable improvement to family practice within the Thai health care system, such as formalization of training and accreditation of family practitioners, along with better pay scales.
Acknowledgments
This research was made possible by a grant from the EC-funded Health Care Reform project (ALA/94/28), contract no. 125.
We are grateful to Ms Supattra Toviriyavej and Ms Tipwadee Tangjitpornkul for their help in organizing the field operations, and Dr Megan Crofts for reviewing the manuscript.
References
1 Nittayaramphong S, Tangcharoensathien V. Thailand. Private health care out of control? Health Policy Planning 1994; 9: 3140.
2 . Tangcharoensathien V, Khongswatt S, Urchaikul C. The diffusion of five medical devices in Thailand in 1995. Bangkok: Health System Research Institute, 1995.
3 Towse A, Mills A, Tangcharoensathien V. Learning from Thailands health reforms. British Medical Journal 2004; 328: 1035.
4 Ahmed AM, Urassa DP, Gherardi E, Game NY. Patients perception of public, voluntary and private dispensaries in rural areas of Tanzania. East African Medical Journal 1996; 73: 3704.
5 Tangcharoensathien V, Bennett S, Khongswatt S, Supacutikul A, Mills A. Patient satisfaction in Bangkok: the impact of hospital ownership and patient payment status. International Journal of Quality Health Care 1999; 11: 30917.
6 Tengilimoglu D, Kisa A, Dziegielewski SF. Patient satisfaction in Turkey: differences between public and private hospitals. Journal of Community Health 1999; 24: 7391.
7 . Utamat P, Nitikawinkul P, Raupornpipat K, Srimakarat S, Tongpon S, Asmongkol S. Suffering because of health care delivery system. (in Thai) Bangkok: The Foundation of Consummer Protection, 1999.
8 Smith HE. Doctors and society: a Northern Thailand study. Social Science and Medicine 1982; 16: 51526.
9 Rakel R. The family physician. In: Rakel, R., ed. Textbook of Family Medicne. Philadelphia: WB. Saunders, 1995.
Table 1 Domains of patient experience covered by the exit surveys
Domain |
Description |
Basic amenities † |
Surroundings with cleanliness, space and ventilation |
Prompt attention ‡ |
Short waiting times |
Communication † |
Clarity of communication, manner of information delivery, willingness to listen to the patient and to |
|
answer patient questions |
Dignity † |
Politeness and respectfulness, not humiliating or demeaning patients |
Trust § |
Confidence in the service received |
† Responses on a 10-point scale from bad to good; ‡ responses on a 4-point scale from very long to very short; § responses on a 10-point scale from very bad to very good in “How well did the doctor examine you?” and yes/no/no idea in “Would you consult here again if you need to see a doctor another time?” and “Would you recommend this doctor to friends or relatives?”
Table 2 Profile of respondents according to sex and type of facilities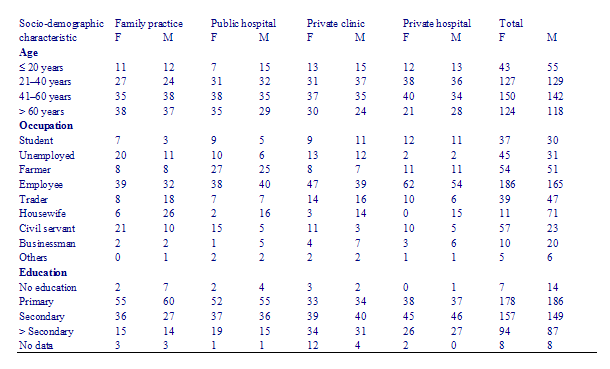
Figure 1 - Differences in score in various domains of patient experience, as provided by patients of family practices and of public hospital outpatient departmentss (*Mann-Whitney U-test: p = 0.001)
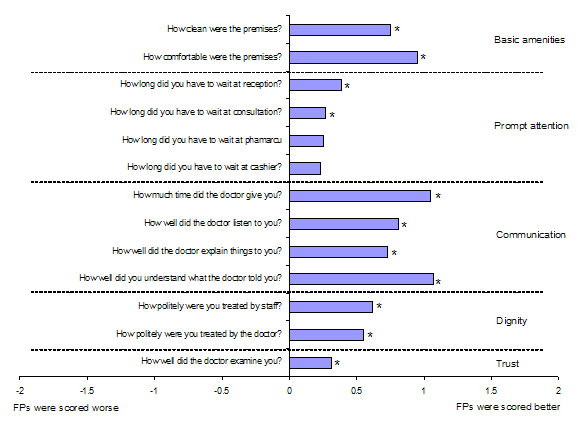
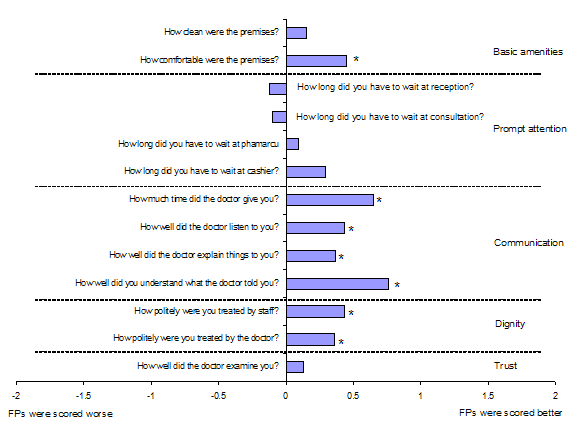
Figure 2 - Differences in score for various domains of patient experience, as provided by patients of family practices and of private clinics (*Mann-Whitney U-test: p = 0.001)