
Training peer counselors in supporting mothers of term, low birth weight infants to exclusively breastfeed
Grace V. Agrasada 1,2 and Elisabeth Kylberg 1
1 Department of Women’s and Children’s Health, Uppsala University, Sweden and 2 Department of Pediatrics, College of Medicine – Philippine General Hospital, University of the Philippines Manila, the Philippines
Methods: An invitation to attend a mother–child health seminar was sent to 13 health centers in Metropolitan Manila. Level One training consisted of a three-day seminar on postpartum mother–child care conducted by the health staff of the Philippine General Hospital. Level Two of the training, conducted by a certified breastfeeding counselor, consisted of a 40-hour instructional program which used interactive didactics and practical skill workshops which taught the counselors how to prevent and manage breastfeeding problems.
Result: Thirty of 37 (81%) women passed Level One training. Fourteen of these 30 women (46.7%) decided to proceed to Level Two training. Eight of the 14 women who had the longest breastfeeding experience were chosen to undergo the Level Two training. All eight women completed the training. Six of the eight (75%) had satisfactory post-training assessment; the remaining two were re-trained and were subsequently assessed to be fit for counseling work. An assessment of post-training competencies showed that counseling knowledge and skills were improved by the training. Further, the intervention demonstrated a 56.6% exclusive breastfeeding rate at six months compared to the national prevalence rate of 1.4%.
Conclusion: This training program has increased breastfeeding counseling knowledge as established by increased correct breastfeeding information and appropriate counseling skills observed after the women completed the training.
Key words: exclusive breastfeeding, breastfeeding counseling training, Manila
Introduction
Face-to-face counseling by peers has been shown to increase breastfeeding initiation,1,2 duration3,4 and exclusivity57 among low-income women and where perinatal breastfeeding support is limited or absent.8 Breastfeeding peer counselors are women who have had positive personal breastfeeding experiences and were trained to support other women in achieving their own breastfeeding goals.
In the Philippines, breastfeeding is promoted mainly by the rooming-in policy9 recommended by the Baby Friendly Hospital Initiative.10 Antenatal services include messages encouraging breastfeeding. Postnatal services, which are principally health center-based, are availed only by 39% of Filipinas11 and do not provide breastfeeding support. Eighteen percent of infants born at term have low birth weight (LBW).12 Based on a longitudinal survey in 198384 in Cebu, Philippines, Adair and Popkin13 concluded that among Filipino infants, LBW decreased the likelihood of being breastfed. However, where mothers opted to breastfeed, being LBW increased the likelihood of being fully breastfed. Fully breastfed was defined as an infant having received less than 20 kcal from supplemental food. Most mothers initiate breastfeeding, but continued exclusive breastfeeding is uncommon. Given the compromised biological status and the poor socio- environmental conditions associated with low birth weight,14 exclusive breastfeeding becomes even more vital for the survival of LBW infants.15
Interventions that address particular concerns about breastfeeding a LBW infant16 and mothers capabilities to sustain exclusive breastfeeding up to 6 months17 would be important. We developed a breastfeeding counseling training program and aimed to test if this training program would enable volunteers to provide information and skilled support to maintain exclusive breastfeeding from birth to 6 months among mothers of term, LBW infants. The counselors trained under this program represented an intervention arm of a randomized controlled trial published elsewhere.18
Method
Counselor selection and training
A two-tiered program was implemented to select and train the counselors. An invitation to a postpartum care seminar was sent to key Local Health Centers in 13 cities of Metro Manila. Figure 1 shows the training framework.
Level One training
The physicians, nurses and midwives of the University of the PhilippinesPhilippine General Hospital conducted a three-day seminar. The content of the training was derived from a postpartum care program for developing countries.19 Maternal care topics covered recognition of postpartum complications (bleeding, pain, foul discharge, fever), preventing breast engorgement, dietary advice, personal hygiene, and contraception. Infant care topics covered warmth, cord care, breastfeeding, growth monitoring and vaccinations. Training materials and snacks were provided at no cost to the participants. A 20-item multiple-choice pretestposttest was conducted to determine the topics where volunteers knowledge was improved by the seminar. The pretest revealed a variation in knowledge of breastfeeding and related topics. About half the group showed satisfactory knowledge in each specific topic. Of those with lack of knowledge in the pretest, all could give correct answers after training in the post-test. Forty active and inactive Barangay (Village) Health Volunteers attended the seminar; 37 of 40 (92%) completed it. The 30 participants with high post-test scores were invited to undergo the next level of training. The principal investigator explained that subsequent training required home visitation. Fourteen of the 30 (47%) were interested to undergo the next level training. The 14 women were ranked according to the duration of personal breastfeeding experience. The top eight women who had the longest breastfeeding experience, an average of 39 months individually, were chosen to undergo the breastfeeding counseling training program. The remaining seven women were to receive general motherchildcare counseling training. Table 1 shows the socio-demographic characteristics of these eight women and the 68 mothers whom they counseled.
Level Two training
This level of training used our own program formulated by modifying widely used training programs20,21 with our own local data and experience. The training emphasized the motherinfant dyad as a unique unit. It was competency-based,22 utilized adult education principles23 and drew on the positive breastfeeding experiences of the counselors. A breastfeeding coordinator, a certified lactation consultant,24 was responsible for the basic and continued training and monitoring of the breastfeeding counselors. The training was conducted in Filipino and covered topics such as home visitation skills, active listening,25 verbal and body language,26 and record-keeping of home visit transactions. Training materials, snacks and transportation to and from the training were provided. The course consisted of 40 cumulative hours over 14 consecutive days of interactive didactics and role-playing.
Didactic interactive sessions
Interactive sessions encouraging participation provided opportunities to practice skills (e.g., role-playing, discussion groups, problem-solving). These sessions were used to facilitate learning of the advantages of exclusive breastfeeding for both infant and mother, assuring the mother that if she decided to breastfeed exclusively, she would be able to do it. Interactive sessions were also used to learn basics of breastfeeding. Particular attention was paid to early feeding cues, handling a physically fragile infant, positioning, and attachment. It was emphasized that mothers need to breastfeed frequently to produce more milk. Milk supply at different lactation stages and infant weight changes over time were thoroughly discussed. How to prevent or manage breastfeeding problems common to Filipino mothers27 were taken up in detail. Counselors were also taught how to understand and cope with divergent views on breastfeeding that family or household members hold. The group developed a semistructured home visitation guide that they used during visits. Table 2 shows discussion topics by day of visit.
Practical skill workshop
By demonstration and return demonstration exercises, the trainees learned how to assist mothers assume a variety of body positions comfortable for breastfeeding. One relevant technique is the Dancer hold position28 where the mother supports babys chin in the sling between her thumb and index finger allowing her a better view and control of her infants head. The counselors learned how to assist mothers in getting more skin-to-skin contact with their infants as this encourages breastfeeding.17 Manual expression of milk, handling expressed milk without refrigeration, and alternative methods of delivering mothers milk to the infant by dropper or spoon were practiced. Family or household members were taught how to do a back rub/back massage on the mother, if the mother would prefer to have one. The counselors were taught how to keep home visit records accurate and up-to-date. Each counselor underwent supervised practice in three different settings: at bedside; at the outpatient clinic; and in the home setting. All eight women who started the breastfeeding counseling training were able to complete the program.
The breastfeeding coordinator monitored all counselors. Counselors attended monthly meetings where breastfeeding counseling training topics were reviewed and individual counseling experiences with mothers were discussed. Additionally, the counselors completed a semistructured home visit form for each mother during each visit. This form contained a structured portion asking about the health conditions of the mother and her infant, breastfeeding problems, if any, and current feeding practice. On the unstructured portion, the counselor wrote her personal feedback regarding the visit. The coordinator collected these forms during monthly meetings.
Eight home visits were scheduled at infant age: Day 35, Day 710; Day 21; at 1.5 months; and then monthly up to 5.5 months. The mothers were asked to bring their infants for the hospital-recommended seven infant-visits at 2 and 4 weeks then monthly until 6 months. These visits were within 2 weeks of each counseling session. At the 6-month visit, a trained, independent interviewer asked mothers individually if and how, their feeding decisions had been influenced during the past 6 months. Additionally, the mothers were asked about their experiences regarding the home visits.
Results
Assessment of training competencies
To assess post-training knowledge, a list of topics (Table 3) was used as a tool. Six counselors were assessed as satisfactory on all topics. The evaluations of two counselors were not satisfactory on three topics, namely: changes in the womans body immediately after childbirth; lactation amenorrhea method;29 and early feeding cues. They were re-trained and when re-assessment was satisfactory, then, they were assigned counseling work. The same tool was used to monitor counselor knowledge on a monthly basis during the entire project.
Counselors feedback on the training
At the end of the program, the breastfeeding coordinator conducted a group meeting and asked the counselors to answer a written training evaluation questionnaire. The evaluation tool had two parts; the first part consisted of a Likert scale; the second part had open-ended questions. Table 4 shows the feedback given by the counselors. All eight counselors stayed on until the end of the trial. All counselors unanimously agreed that the learning and experience from counseling had built up their self-esteem and increased their self-confidence. The mothers, including those who failed to exclusively breastfeed up to 6 months said that they were satisfied with the counseling they received.
Mothers feedback
At exit interview, all mothers who had received home-based counseling stated that they were satisfied with the counseling they received. Mothers in the breastfeeding group believed that the counselor influenced their feeding decisions the most. None of the mothers requested counselor replacement. During the 6th month infant hospital visit, a trained interviewer asked the mothers what they thought about the peer counseling they received. Table 5 shows the opinions of mothers on how the counseling program supported the mothers.
Breastfeeding practice
The breastfeeding coordinator collected breastfeeding practice reports from the counselors logbooks. At infant ages week 2, 8, 16 and 24, the proportion of mothers who were exclusively breastfeeding were as follows: 76.4% (52/68), 72.5 (45/62), 61.6% (37/60) and 56.6% (34/60), respectively. The decreasing denominators indicated the number of withdrawals (mothers relocated outside study area) or mothers who decided to stop breastfeeding. Eighty seven percent (59/68) of mothers received all eight visits. Thirteen-percent (9/68) of mothers were unable to complete the counseling program. One mother decided to stop breastfeeding completely and eight mothers relocated. Before relocation, two 4-week-old and one 8-month-old infant were breastfed exclusively. Four mothers combined breastfeeding with formula.
Discussion
This training program has increased the knowledge and skills of low-income, peer volunteers in breastfeeding counseling. This had been established by increased correct breastfeeding information shown on assessments and appropriate counseling skills observed after the women completed the training. The mothers stated that most of their breastfeeding problems were prevented or solved by counseling they received. The effectiveness of the training was further validated by the increased exclusive breastfeeding prevalence rate of 56.6% at 6 months compared to the national prevalence rate of 1.4%. Careful selection of counselors and their continuous, appropriate training, generated correct breastfeeding information and provided skilled, practical support to mothers. The satisfactory outcomes can be attributed to proper training and the counselors dedication to their training. The motivation to learn had been demonstrated by all counselors having completed the training. The mothers stated that most of the breastfeeding problems were prevented or solved by counseling. Even those mothers who opted to breastfeed, but not exclusively at certain instances, continued to appreciate counseling as this helped them continue breastfeeding. Problems occurring along the breastfeeding period like breast engorgement, poor milk supply and poor infant weight gains, were recognized. The counselors worked with the mothers to solve problems. Repeated information and skills practiced frequently increased counselors competencies. The commitment to counseling work was reinforced by constructive feedback, from the breastfeeding coordinator, co-counselors, and mothers. Not living in the same community was not a disadvantage in this home-based program. Mothers appreciated that peers with training and skills helped them on issues that were important to them.
Our findings are consistent with earlier studies showing that training improved breastfeeding knowledge and skills. Rea and co-workers documented the effectiveness of the WHO/UNICEF 40-hour course among health workers in Brazil.30 The same course was used to train volunteers in a successful breastfeeding peer counseling program in Bangladesh.31 Similar results were found among health workers in Nigeria who used an 18-hour UNICEF training program.32
The women who volunteered to undergo training in this study had the advantage of having positive personal experiences and this may have contributed to how well they received the training. The two-level training enabled us to identify the topics, which demanded more focus in the breastfeeding counseling program. Our training process prevented attrition by using a training-retraining cycle; hence, all volunteers entered into the counseling work when they were ready, which implied strength in the skill of counseling.
By combining what was relevant and appropriate in breastfeeding training courses to our own local experience, we have developed a peer counseling training program that prepared volunteers to successfully support mothers who would like to exclusively breastfeed their LBW infants from birth to 6 months.
Summary of implications for practice
1 Family physicians should be able to promote, protect, and support breastfeeding. It is important that health professionals and lay volunteers have defined roles and collaborate to achieve common breastfeeding goals.
2 Peer counseling may be an essential component of any breastfeeding promotion program and can be most useful when integrated into the primary care level of health services. Careful selection of trainees, and training appropriate to local experiences, will ensure successful peer counseling training programs.
Acknowledgments
This publication was supported by InDevelop, the Swedish Institute, Sida, Uppsala University and the University of the Philippines Manila. We would like to thank the eight women volunteers and the mothers who participated in this study. We appreciate the feedback on the training program by Professor N Fajutagana, National Teachers Training Center, University of the Philippines Manila.
References
1 Ahluwalia IB, Tessaro I, Grummer-Strawn LM, MacGowan C, Benton-Davis S. Georgias breastfeeding promotion for low-income women. Pediatrics 2000; 105: 85.
2 Shaw E, Kaczorowski J. The effect of a peer counseling program on breastfeeding initiation and longevity in a low-income rural population. Journal of Human Lactation, 1999; 15: 1925.
3 Schafer E, Vogel MK, Viegas S, Hausafus C. Volunteer peer counselors increase breastfeeding duration among rural low-income women. Birth: Issues in Perinatal Care, 1998; 25: 1016.
4 Gross SM, Caulfield LE, Bentley ME et al. Counseling and motivational videotapes increase duration of breast-feeding in African-American WIC participants who initiate breast-feeding. Journal of the American Diet Association, 1998; 98: 1438.
5 Kistin N, Abramson R, Dublin P. Effect of peer counselors on breastfeeding initiation, exclusivity, and duration among low-income urban women. Journal of Human Lactation 1994; 10: 115.
6 Morrow AL, Guerrero ML, Shults J et al. Efficacy of home-based counseling to promote exclusive breastfeeding: a randomised controlled trial. Lancet, 1999; 353: 122631.
7 Haider R, Ashworth A, Kabir I, Huttly SR. Effect of community-based counselors on exclusive breastfeeding practices in Dhaka, Bangladesh: a randomised controlled trial. Lancet, 2000; 356: 16437.
8 Arlotti JP, Cotrell BH, Lee SH, Curtin JJ. Breastfeeding among low-income women with and without support. Journal of Community Health Nursing, 1998; 15: 16378.
9 Department of Health. The National Objectives for Health, 19992004. Manila: Department of Health: 1999.
10 World Health organization. Protecting, promoting and supporting breastfeeding. The special role of maternity services. A joint WHO/UNICEF statement. Geneva: WHO, 1989.
11 Republic of the Philippines. National Health and Demographic Survey. Manila: National Census Office, 1998.
12 UNICEF. The Official Summary of the State of the Worlds Children 2003. New York: UNICEF, 2002.
13 Adair LS, Popkin BM. Low birth weight reduces the likelihood of breast-feeding among Filipino infants. Journal of Nutrition, 1996; 126: 10312.
14 Kramer MS. Determinants of low birth weight. methodological assessment and meta-analysis. Bulletin of the World Health Organization, 1987; 65: 663737.
15 Arifeen S, Black R, Antelman G, Baqui A, Caulfield LE, Becker S. Exclusive breastfeeding reduces acute respiratory infection and diarrhea deaths among infants in Dhaka slums. Pediatrics, 2001; 108: E67.
16 Kavanaugh K, Mead L, Meier P, Mangurten HH. Getting enough: mothers concerns about breastfeeding a preterm infant after discharge. Journal of Obstetrics and Gynecological Neonatal Nurs, 1995; 24: 2332.
17 World Health Organization. Global Strategy for Infant and Young Child Feeding. Geneva: WHO, 2003.
18 Agrasada GV, Gustafsson J, Kylberg E, Ewald U. Postnatal peer counseling on exclusive breastfeeding of low birth weight infants: a randomized, controlled trial. Acta Paediatrica, (Accepted for publication November 2004.)
19 Savage F, Daelmans B. Training health care workers to counsel breastfeeding mothers. Dialogue Diarrhoea 1995: 2.
20 World Health Organization. Breastfeeding Counseling. A Training Course. Geneva Division of Diarrhoeal and Acute Respiratory Disease Control: WHO/CDR/93 36 UNICEF/NUT/, 1993, 93, 14.
21 King FS. Helping Mothers to Breastfeed. Revised ed. Nairobi: African Medical and Research Foundation; 1992.
22 Chambers DW, Ed M. Toward a competency-based curriculum. Journal of Dentistry Educ, 1993; 57: 7903.
23 Roger A. Teaching Adults. Milton Keynes: Open University Press, 1986.
24 Kelley KJ. Accountability: the IBLCE discipline process. International Board of Lactation Consultant Examiners. Journal of Human Lactation, 1999; 15: 612.
25 Decker B. The Art of Communication. USA: Crisp Publications. 1988.
26 Axtell RE. Gestures The Dos and Taboos of Body Language Around the World. New York: John Wiley & Sons, 1991.
27 Guthrie GM, Guthrie HA, Fernandez TL, Estrera N. Early termination of breastfeeding among Philippine urban poor. Ecology of Food Nutrition, 1983; 12: 195202.
28 Lang S. Breastfeeding Special Care Babies. London: Ballière-Tindall. 1997.
29 Perez A, Labbok MH, Queenan JT. Clinical study of the lactational amenorrhoea method for family planning. Lancet, 1992; 339: 96870.
31a Rea MF, Venancio SI, Martines JC, Savage F. Counseling on breastfeeding. Assessing knowledge and skills. Bulletin of the WHO, 1999; 77: 4927.
30 Haider R, Kabir I, Huttly S, Ashworth A. Training peer counselors to promote and support exclusive breastfeeding in Bangladesh. Journal of Human Lactation, 2002; 18: 712.
31 Davies-Adetugbo AA, Adebawa HA. The Ife South Breastfeeding Project: training community health extension workers to promote and manage breastfeeding in rural communities. Bulletin of the World Helath Organization, 1997; 75: 32332.
Fig. 1 The breastfeeding counseling training framework.
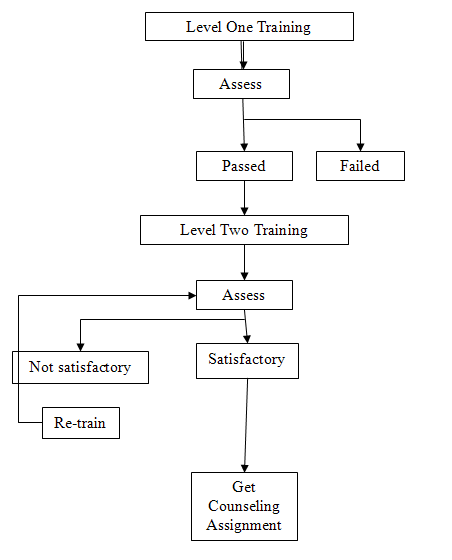
Table 1 Selected characteristics of breastfeeding counselors and the mothers who received counseling.
Characteristic |
Counselors |
|
Counseled mothers |
|
|
n = 8 |
% |
n = 68 |
% |
Mean (SD) age, years |
37.9 (5.9) |
|
22.7 (4.5) |
|
Living in Manila |
3 |
37.5 |
22 |
32.4 |
Living with husband/partner |
8 |
100 |
61 |
89.7 |
Work/study outside home |
3 |
37.5 |
18 |
26.5 |
Formal education, in years: |
|
|
|
|
Less than 10 |
1 |
12.5 |
19 |
27.9 |
10 or more |
7 |
87.5 |
49 |
72.1 |
Mean (SD) annual income, US$ |
1343 (102) |
|
1358 (126) |
|
† Per cent unless stated otherwise
Table 2 Topics discussed by peer counselors with mothers on home visits
Infant age |
Topics |
Days 3–5, 7–10, 21–23 |
Mother’s well being (feelings, sleep, rest, ambulation) |
|
Danger signs (maternal pain, bleeding, foul discharge, fever) |
|
Mother’s postpartum hospital check |
|
Breast engorgement, breast pain, nipple condition |
|
Infant’s condition (warmth, color, sleep, voiding, stools) |
|
Breastfeeding (positioning, attachment and increasing milk supply) |
|
Infant medical check including vaccination |
|
Infant weight changes |
Week 6, 10 |
Mother’s well being and sexual activity |
|
Mother’s child spacing choice |
|
Requirements and benefits of lactation amenorrhoea method |
|
Work/study outside the house |
|
Infant medical check and vaccination |
|
Infant’s health and growth |
|
Breastfeeding situation |
|
Milk expression, storage and how to feed expressed milk to infant |
Week 14,18, 22 |
Mother’s well being, child spacing |
|
Work/study outside the house (handling expressed milk) |
|
Infant medical check and vaccination |
|
Infant health and growth |
|
Breastfeeding situation |
|
Advice on timely complementary feeding |
Table 3 Breastfeeding training topics on which the counselors were evaluated
What happens to a woman’s body after infant delivery? |
What happens to a baby immediately after birth? |
How can a mother breastfeed a LBW infant? |
How can a mother breastfeed of LBW infant exclusively from birth to 6 months? |
Why is exclusive breastfeeding good for mothers? |
Why is exclusive breastfeeding good for infants, particularly for those born with LBW? |
Which are the early feeding readiness cues? |
Which signs show that the infant is having a good attachment and positioning ? |
Which signs show that breastfeeding is going well? |
How much should a breastfeeding infant weigh? |
What are the infant voiding/stool patterns when breastfeeding is going well? |
What would you advice mothers when an infant refuse the breast? |
What would you advice mothers when an infant is too sleepy to feed? |
What are the requirements and benefits of Lactation Amenorrhoea Method (LAM)? |
How does a mother increase her milk production? |
How does a mother introduce timely complementary feedings? |
Table 4 Counselor feedback on the training they received
Questions |
Strongly agree |
Agree |
Disagree |
Strongly disagree |
Were the training objectives met? |
8/8 |
|
|
|
Were the issues I want to know addressed? |
7/8 |
1/8 |
|
|
Were the training materials helpful, clear? |
8/8 |
|
|
|
Was the schedule/duration of the training acceptable? |
6/2 |
2/8 |
|
|
Was the teaching style clear and organized? |
8/8 |
|
|
|
Was participation in the discussion encouraged? |
8/8 |
|
|
|
How would you like to improve the training No answers What aspects of the training did you like best? All of it (2/8) The training considered our cultural ways. (2/8) All of it; specifically the chance to re-train those who did pass the first assessment (2/8) All of it, including the fact that we were few in our group (1/8) I like it when we were able to prepare a home visit guide that we all found useful during homevisits. (1/8) |
||||
Additional Comments The training gave me new knowledge and skills – I feel good about the training (8/8) I enjoyed the training because I found new friends (5/8) I am proud to be trained by the hospital staff (8/8) |
||||
Table 5 The mothers feedback about peer-counseling program
Question |
% |
Who influenced you most regarding feeding decisions the past six months? |
|
Counselor |
91.7 |
Counselor and husband |
5.0 |
Counselor and mother |
3.3 |
Why do you like peer counseling program? |
|
“… I did not have to spend for it …” |
91.6 |
“… helped me look after my own health ….” |
83.3 |
“…helped me decide how to feed and care for my baby …” |
41.7 |
“The counselor”s visit was for everyone in my house, even my neighbors come to listen.’ |
13.3 |
“Convenient. I do not have to travel …” |
11.7 |
“The counselor discussed with my husband and mother-in-law how they could help me” |
5.0 |
“… she (counselor) listens to my other (non-breastfeeding) problems” |
3.3 |
“It was nice to expect someone to come as agreed…” |
3.3 |
‘… she did not force me to breastfeed exclusively. She continued even if I decided to supplement. |
3.3 |
Do you like the peer counseling program? |
|
Yes |
100 |
No |
0 |
The number of visits |
|
Few |
8.3 |
Just right |
91.7 |
Too frequent |
0 |
The duration of the visits |
|
Too quick |
16.7 |
Just right |
83.3 |
Too long |
0 |
^top