ORIGINAL
ARTICLE
What are the barriers faced by doctors
in the management of erectile dysfunction in general practice?
Ngiap
Chuan TAN,1 Chirk Jenn NG,2 Wah Yun LOW,3
Wan Yuen CHOO3 
1College of Family Physicians, Singapore, 2Department of Primary
Care Medicine and 3Health Research Development Unit, Faculty of Medicine,
University of Malaya, Kuala Lumpur, Malaysia
Aim:
This study was conducted in Singapore and aimed to determine
the barriers perceived by general practitioners (GPs) in the
management of their patients with erectile dysfunction (ED).
Methods: This was a qualitative analysis of a sample
of 22 GPs using focus group discussions. Data were analyzed
using content analysis techniques.
Results: Erectile dysfunction as a problem was often
hidden in the agenda during GP-patient consultations. GPs perceived
that older patients accepted ED as part of the ageing process
but that for younger patients, GPs attributed fatigue as the
etiology of ED. GPs felt that most patients preferred using
widely publicized medications for ED, as a quick solution for
their problem, rather than undergoing a thorough evaluation
of the problem. Costs of medication for ED was constantly highlighted
by GPs as a barrier to effective management, although some regarded
it as a deterrent to social and moral degradation. Side-effects
and improper administration of the medication were problems
raised by GPs. Barriers included: the GP's gender; competence;
perception of ED as less critical compared to the patient's
comorbidities; and a passive approach to the problem. Relevant
training and a good doctor-patient relationship were considered
as likely to improve the management of ED.
Conclusions: Interplay of doctor, patient and drug factors
needs to be addressed to enhance the management of ED. Understanding
of this interaction will enable GPs to be proactive in their
approach, diagnosis and treatment of ED.
Key
words: barrier, erectile dysfunction, general practitioners,
Singapore
Introduction
In Singapore over the past three decades, vast socio-economic improvement
has had a significant impact on the lifespan and lifestyle of its
citizens. The ageing population contributes to the rising prevalence
of chronic ailments such as hypertension and diabetes mellitus. Both
these chronic diseases and age can adversely affect sexual function.
Sexual matters such as erectile dysfunction (ED) used to be a taboo
subject. With the advent of the information revolution, media publicity
and the availability of effective oral medication for erectile dysfunction,
general practitioners (GPs) recognized that the subject was being
raised more with their male patients. The subject is not unique to
any race and religion in multiracial Singapore. Similar findings were
detected in a study1 in neighboring Malaysia, where the population
consists of a similar mix of Asians including Malays, Chinese, Indians
and Eurasians.
Nonetheless, the management of ED is hindered by a complex interplay
of doctor, patient, medication and socio-cultural factors. Another
Malaysian study2 has highlighted problems faced by GPs in ED treatment
but there has not been a similar report from Singapore. This study
aims to identify and explore the various factors that impede effective
ED management in general practice in Singapore.
Methods
The study population included GPs practicing in both private clinics
and government-aided primary care centers in Singapore. Participants
were purposively recruited, based on the inclusion criterion that
they had managed patients with ED and had instituted treatment for
ED. The GPs were invited through personal contact, introduction letter
via the post or email, which clearly stated the objectives of the
study.
This study utilized focus group discussions to obtain in-depth information.
Focus groups are an accepted way to explore knowledge and experiences,
and examine not only what people think, but how and why they think
in a particular way.3 However, it does not provide quantitative data
that can be generalized to the wider population.
The focus groups were carried out at a local clubhouse and a clinic,
and were facilitated by the first two authors (Tan and Ng) based on
a structured discussion guideline. The guideline covered the following
topics:
-
GPs'
attitudes and perceptions toward ED and its treatments;
-
managing
ED in their practice;
-
prescribing
habits and assessment of new ED treatments.
Written
consent was obtained from each participant, who also provided basic
socio-demographic data in a questionnaire. Each focus group session
was audio-taped and lasted approximately 90 minutes. Detailed notes
of each session were taken. The study was terminated with saturation
of ideas after four such sessions. The tape-recorded interviews were
transcribed in their entirety into text files.
This
qualitative data were analyzed using standard content analysis technique,
which allowed valid inference to be made from the text by extracting
patterns of themes in the data.4
All transcripts were read and checked several times to ensure consistencies
and were coded according to potential conceptual and content-related
themes, using a qualitative data analysis software NUD*IST Version
6.0.5
The quotes were typical views expressed by the GPs to exemplify emergent
themes.
Results
Socio-demographic background of participants
The participants comprised 22 GPs, aged from 26
years to 56 years with a mean age of 34.8 years (SD = 5.6 years).
The participants generally treated an average of four ED patients
per month. Half of them had attended workshops or seminars related
to sexuality. The profiles of the GPs are listed in Table
1.
Factors influencing the management of ED are presented in themes from
various perspectives, namely factors related to patient, doctors and
drugs (Table 2).
Patient
factor
GPs felt that the majority of patients were silent sufferers of ED.
Most of these men did not volunteer that this was a problem, or had
difficulty bringing up the subject to their GPs. Obtaining a history
of ED was often not straightforward and required GPs to dig out such
'secrets'. Decoding this secret was a test of the skills of the GPs
as patients presented the problem in myriad ways. GPs frequently discovered
that the ED history was 'hidden' in the main agenda of the consultation.
Others used a second party to bring up the topic.
An ED information pamphlet in the clinic is another tool that subjects
utilize to bring their GP's attention to their problem.
Patients would make use of their medications to bring up the topic
and commonly queried if ED is the consequence of side-effect of their
regular long-term medications. One GP claimed he detected a case of
ED from a patient with failure to consummate a marriage.
The surge in emotion from their patients during the consultation could
pose a problem for the GPs if they were ill-prepared to handle it:
'…they start talking …sometimes can be quite emotional,
very trapped in that sense… being very frustrated; the wife can
become quite, rather dissatisfied; …anytime, when they are about
to do it, and you cannot get it to stand, the wife …vow, the
expression is there…they felt that they are quite inadequate.'
A lag time was common before the problem finally surfaced to the GPs.
During the interim period, GPs perceived that self-medication with
traditional herbs was characteristic of help-seeking behavior of local
men.
However, this traditional barrier was viewed by the GPs as disintegrating
with increased media coverage and publicity of the problem and its
pharmaceutical treatment. 'I agree with what (GP) had said, generally
they (men in general) are now more frank, their erectile dysfunction
…now that this medicine is available, I don't think that any
of them are shy about it.'
In fact, the trend was perceived to move to the other extreme. Increasing
numbers of men would directly ask their GPs to prescribe the anti-ED
drug as a quick fix treatment rather than solve the problem.
As such patients preferred this short-circuit approach to the problem,
GPs encountered difficulty in getting them to undergo a full assessment,
as indicated by the Singapore Urological Association guidelines for
ED management. From the patient's perspective, they would prefer to
simply take the medication without further evaluation and possibly
avoid additional cost from the investigations. 'The difficulty will
be to convince the people who are seeking treatment to undergo the
full assessment …who …among our patients are willing to
succumb themselves to all these tests?'
The GPs also encountered men seeking medication for ED from another
physician rather than from their regular GP, to avoid embarrassment
and to hide their ED problem. 'I have a lot of husbands who come and
see me because they don't want to go to their regular family doctor
for their Viagra …they feel that …the regular doctor will
not keep their secret for them or they felt a bit "pai seh"
(embarrassed) about it.'
Medication factor
The availability of an oral form of anti-ED medication was a step
forward in ED management. Despite a more acceptable form of therapy
for men in comparison to hitherto parenteral and inflatable devices,
drugs for ED have their own set of potential problems.
The cost of the medication was repeatedly highlighted in all the focus
group sessions as a prime consideration among GPs in the management
of ED. The GPs felt it could deter those from the lower socio-economic
strata of society. The high cost might possibly prompt users to seek
them at cheaper prices in the 'black market' but at the risk of acquiring
adulterated medication of unknown quality and without proper instruction
for its administration.
However, one GP argued that the cost of the drug was a matter of relativity.
It depended on the perceived personal values and attitude of the patient.
If sexual function constitutes a vital part of a person's life, cost
of treatment will be secondary. 'Cost is not a problem …it reflects
the importance of this aspect of life. I felt that it's very important,
in fact, sex is very important. So they don't mind spending.' In contrast,
several GPs considered the price of drug treatment acted as a deterrent
to social and moral decadence. In fact the drug has opened up a new
horizon for men with ED that the pendulum has now swung to the other
end, with people using it as a recreation drug.
Some GPs were at odds with themselves as they felt they had an obligation
to safeguard the men's spouses and ultimately the morality of society.
GPs gave examples of family relationship breakdowns in the advent
of the medication for ED.
According to the GPs, press reports of death associated with sildenafil
(Viagra) dealt a blow to the confidence of potential users, although
the direct link was not fully established. This was one reason for
men with ED to try out their familiar herbs and traditional medications,
which were of variable and often not proven efficacy, instead of consulting
their GP for ED management.
The 'failure' of sildenafil to treat ED due to improper administration
such as immediate ingestion just prior to coitus also had an adverse
impact on the user.
The myth that sildenafil was used as an aphrodisiac could result in
failure to resolve the ED problem.
Certain patients might also shun the drug as they experienced the
side-effects from the therapy, though most were self-limiting and
not life-threatening. 'The difficulty is the side-effects. Sometimes
they do get a bit of side-effects like giddiness or headaches or nasal
congestion.'
Physician
factor
The GPs also felt that elderly men were more concerned about comorbidities
and regarded ED as part of their ageing process.
In contrast, several GPs felt that the younger patients' poor sexual
performance could be related mainly to factors such as fatigue rather
than ED itself.
Failure of the GPs to consider ED as a disease in either group of
men would deter detailed exploration of the problem.
The gender of the GP seemed to influence the decision of men to raise
the topic of their ED. The GPs perceived that the presence of male
doctors was advantageous, as men tend to highlight the problem to
male more than female doctors. Female GPs were also less likely to
bring up the subject for fear of distorting their 'lady' image and
misconceived ideas by the male ED sufferers.
More patients tend to open up if they perceived that their GPs were
confident of treating such problems or more proactive in their approach
to managing ED. A good patient-doctor rapport is another key factor
to bring out the problem.
The GPs seldom raised the problem routinely. They would deal with
ED only after the patients brought up the topic themselves or after
adequate rapport was established after a series of consultations.
They were concerned and apprehensive to initiate the discussion of
sexual dysfunction themselves, lest they triggered an unpleasant reaction
from their patients.
GPs were more willing to query the effect of ED for male patients
with chronic illnesses and medications associated with ED, such as
diabetes mellitus and hypertension. They were unlikely to raise the
subject for patients who came for acute ailments such as flu and diarrhea,
to avoid perceived ridicule by their patients.
However, GPs occasionally faced restraint in their attempt to switch
certain blood pressure lowering medications with known deleterious
effect on erectile function. Patients ultimately would be the decision
maker. 'If they are very comfortable with atenolol, they don't want
to change …there is only this much you can do …sometimes
they would rather go ahead with their (usual) medication …(patient
says) don't have any side-effect from the high blood pressure or diabetes.
Just give me another medicine to help me with my ED.'
Most GPs considered themselves as 'passive prescribers' of anti-ED
medication on a case-encounter basis. They would be more willing to
prescribe if they detected actual cases of ED.
In contrast, a few GPs did not prescribe medication for ED as they
lacked confidence. Another GP sent patients to the urologist for the
initial workup and would then continue the ED medication if the urologist
commenced such therapy.
In general, GPs would adopt a reactionary approach, as and when patients
presented the problem to them. This was especially so with new patients
when rapport was yet to be established.
Training and confidence go hand-in-hand in the management of ED in
primary care. The study showed that GPs with training in relevant
fields, such as andrology, were more proactive in dealing with ED.
With background training in andrology, one GP considered 'ED as a
barometer of cardiovascular health' as 'artherosclerosis would definitely
affect the penis'. He would actively pose the question: 'How's your
sexual health?' to all his patients, especially those above 40 years
and with comorbidities such as diabetes mellitus and hypertension.
However, another GP in the same setting retorted that: 'ED is a barometer
of vascular disease… don't you think it's a late-stage event!'
It perhaps reflected GPs' variable perceptions of ED in terms of urgency
and importance as a disease.
Several GPs had prescribed drug treatment for ED and then discovered
that the patients were using them in extra-marital relationships.
One GP felt strongly that he should not be promoting promiscuity.
However, the general sentiments were that GPs should not be judgemental,
though a few tried hard to reconcile their roles as both a physician
and a stakeholder of social and moral responsibility.
The GPs felt that if a patient came with a fixed mindset to obtain
treatment for ED and nothing else, they would usually comply after
ruling out any contraindications. They were well aware that these
patients would obtain drugs elsewhere if they did not prescribe.
Ultimately the GPs felt that the onus to take the medication for ED
remained with the patients themselves.
Discussion
The study showed an interplay of factors that potentially could have
an impact in ED management in general practice. Most GPs in the study
felt that social stigma was still a hindrance to the presentation
of ED, leading to inadequate exposure of the problem in general practice.
Common barriers included men wanting to avoid revealing their inadequacy
and avoid embarrassing both their sexual partner and their GP. GPs
were aware of patients' different, and often subtle, presentations
of ED but they needed to take the initiative to raise the problem
during the consultation and to handle the occasional vehement emotions
from their patients. Their perception that older men's acceptance
of ED as an ageing process and attributing fatigue as the predominant
cause of ED in younger men, would hinder detailed exploration of the
problem.
However, GPs also noted the evolving pattern of ED presentation with
gradual dissolution of such inhibition among the affected patients.
The gradual opening up of this inhibition may not necessarily translate
into more effective ED treatment. The authors felt that the walk-in
system of primary care in Singapore allowed patients to doctor-hop
and seek treatment and medication in different clinics. This fragmented
care would hamper the overall ED management as the 'new' GPs were
disadvantaged by their possible lack of familiarity with the patients'
other medical conditions and family background.
The pay-for-service system in the local context is regarded as another
hurdle. Cost of medication is added to the service at the GP clinics,
which also coupled as a dispensary, unlike in the West where drugs
are dispensed at the pharmacy. Patients pay full cost for the medication
or devices for treating ED. It added on to the overall cost of treatment
of their chronic diseases.
Cost of medication was perceived by the GPs to have contradictory
effects. For men who needed the drug for their ED, the cost could
be forbidding for those from the lower socio-economic class. On the
other hand, GPs regarded cost to be a deterrent to rampant abuse.
Failure to adhere to proper administration of the current drug for
ED, side-effects and tainted reports of adverse reactions in the media,
were other factors which hindered the pharmacological management of
ED.
It was also not surprising that GPs encountered patients' reluctance
to undergo full investigations for ED, perhaps as a cost-saving measure.
It eroded the confidence of the GPs in managing these patients, not
only for safety reasons, but also because of medico-legal considerations.
Read et al.6 noted that many men considered sexual issues to
be an appropriate subject for the GP to discuss. Despite this, only
2% of the GPs' notes showed records of sexual problems.6 A study of
healthcare needs in the general population had indicated that only
a small proportion of patients wanting professional help for sexual
problems actually receive it.7 In fact, many preferred doctors to
initiate discussion on sexual issues related to their medical
condition.1
For those who seek treatment, there was a delay of about one year
between the onset of the problem and presentation of the complaint
of ED to the GPs by patients.
The study revealed that GPs' lack of proactive approach to ask about
ED in their patients could be one possible answer. The fact that ED
did not manifest proportionate to its prevalence was partially attributed
to GPs' attitudes, passive approach, competence and confidence in
dealing with the problem. The GPs' passive approach might be shaped
by their attitude that regarded ED as less critical to treat than
other comorbidities. They also feared that their image could be tarnished
if they were perceived to be promoting medication for ED.
Many GPs in the study regarded the treatment of the chronic diseases
to take precedence over the management for sexual function, which
was lower down in their priorities. The treatment of a perceived 'non-urgent'
condition could adversely influence the GPs' decision to initiate
ED discussion with their patients.
Although physicians are the most frequently consulted professionals
for sexual problems, it has been suggested that they are often ill-prepared
to handle these problems.8,9 This was illustrated by the two GPs in
this study who tended not to prescribe drugs for ED because they were
'not confident'.
The results were comparable to that of Low's study2 where the constraints
identified by GPs in dealing with sexual problems included:
- lack
of training and knowledge on sexual problems;
- being
the opposite sex to their patients; and
- the
fear of offending patients.
However,
time constraint was not mentioned as a factor in this study.
In
addition, the GPs' prescribing behavior was influenced by the patients'
pattern of presentation and request for medication.10 They struggled
to reconcile their dual roles as a 'healer' of their patient's ED
problem and a guardian against moral and social decadence resulting
from prescription of anti-ED medication. The issue of diagnosis and
treatment of ED, like many other chronic diseases, involved a complex
interplay of factors.11
Training
in sexual health for relevant disciplines could perhaps inject confidence
in the prescribing of medication for ED as exemplified by the andrology-trained
GP. In addition, experience and the traditional skills of GPs in establishing
good rapport with their patients are catalysts toward holistic management
of their patients with ED.
Conclusion
The study showed that patient, medication and doctor factors could
adversely affect the management of ED. These issues need to be addressed
and a better understanding of how these factors interact is important
in order for ED to be adequately treated in general practice.
Acknowledgments
The authors wish to extend their thanks to Dr Wong TKM for his assistance
and the participating general practitioners for their contribution
to the study. The study was supported by an educational grant from
the Asia Pacific Society for Sexual and Impotence Research (APSSIR)
and GlaxoSmithKline Pharmaceutical and Bayer Healthcare.
References
| 1 |
Low
WY, Wong YL, Zulkifli SN, Tan HM. Malaysian cultural differences
in knowledge, attitudes and perceptions related to erectile dysfunction:
focus group discussion. Intern. J. Impot
Res. 2002; 14: 440-5. |
| 2 |
Low
WY, Khoo EM, Tan HM. Sexual Health Problems:
Attitudes and Practices of Malaysian General Practitioners.
Auckland: Adis International Ltd, 2002. |
| 3 |
Kitzinger
J. Introduction to focus group discussion. Br.
Med. J. 1995; 311: 299-302. |
| 4 |
Palton
M. Qualitative Evaluation and Research
Methods. Newbury Park, CA: Sage Publications, 1990. |
| 5 |
Richard
T. N6 Reference Guide. Melbourne:
QSR International Pty Ltd, 2002. |
| 6 |
Read
S, King M, Watson J. Sexual dysfunction in primary medical care:
prevalence, characteristics and detection by the general practitioner.
J. Public Health Med. 1997;
19: 387-91. |
| 7 |
Dunn
KM, Croft PR, Hackett GI. Sexual problems: a study of the prevalence
and need for health care in the general population. Fam.
Pract. 1998; 15: 19-24. |
| 8 |
Pauly
IB, Goldstein SG. Physicians' ability to treat sexual problems.
Med. Aspects Hum. Sex 1970;
4: 24. |
| 9 |
Broekman
CP, van der Werff ten Bosch JJ, Slob AK. An investigation into
the management of patients with erection problems in general practice.
Int. J. Impot. Res. 1994;
6: 67-72. |
| 10 |
Morgentaler
A. Male impotence. Lancet
1999; 354: 1713-8. |
| 11 |
Greenhalgh
T, Gill P. Pressure to prescribe. involves a complex interplay
of factors. Br. Med. J. 1997;
315: 1482-3. |
Table
1 Socio-demographic background and
practice profile of participating GPs in Singapore
| Variable |
Frequency
n = 22 |
Percentage |
Mean
(SD) |
| Age |
|
|
|
| <
35 |
11
|
50.0 |
34.8
(5.6) |
| 35-55 |
10 |
45.5 |
|
| >
55 |
1 |
4.5 |
|
| Ethnic
group |
|
|
|
| Chinese |
22 |
|
100.0 |
| Sex |
|
|
|
| Male |
18
|
|
81.8
|
| Female
|
4
|
|
18.2 |
| Religion |
|
|
|
| Buddhist |
2 |
|
9.1
|
| Christianity |
14
|
|
63.6 |
| Others |
6 |
|
27.3 |
| Marital
status |
|
|
|
| Single
|
2 |
|
9.1 |
| Married
|
20 |
|
90.9 |
|
Classification
of practice
|
| Government |
5 |
|
22.7 |
| Private |
17 |
|
77.3 |
|
Types
of private practice (n = 17)
|
| Single
doctor |
9 |
|
47.1 |
| Group |
8 |
|
52.9 |
|
Number
of years practicing medicine
|
| <
10 |
10 |
45.5
|
9.8
(5.5) |
| =
10 |
12 |
54.5 |
|
| Number
of patients treated for ED (per month) |
| <
1 |
2 |
9.1 |
4.0
(9.1) |
| 1-4 |
16 |
72.7 |
|
| >
4 |
4 |
18.2 |
|
| Number
of years prescribing anti-impotent oral treatment |
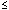 3 3
|
20 |
90.0 |
2.2
(1.3) |
| >
3 |
2 |
10.0 |
|
| Attended
workshop on sexuality |
| Yes |
11 |
50.0 |
|
| No |
11 |
50.0 |
|
back
to text
Table
2 Themes
emerged from the focus groups
|
Factors
|
Themes |
| Patient |
GP
perceived that patients often hid their ED and were often not straightforward
in their presentation.
GP encountered patient's reluctance to full assessment of ED.
Cost of anti-ED medication was widely regarded as a deterrent |
| Medication |
Improper
administration and side-effects could deter the patient from using
the drug
GP's gender, perceived competence and passive approach to the problem
were perceived as barriers in ED management. |
| Doctor |
Relevant
training and good rapport with patient could overcome the barriers.
GP perceived older men's acceptance of ED as an ageing process and
attributed fatigue as a predominant cause of ED in younger
men. |
back
to text
|
![]()
